Last Updated on July 18, 2023 by Nurse Vicky
Unraveling the Mystery: Why is Malaria More Prevalent in Africa than Other Parts of the World?
Malaria, one of the most significant health challenges worldwide, poses a particularly pronounced threat in Africa. Despite substantial efforts in disease control, this fatal malady remains entrenched in this part of the world.
This comprehensive guide delves into the intricate layers of the malaria issue in Africa, exploring its prevalence, contributing factors, and potential solutions.
Understanding Malaria
Before delving into why malaria is more common in Africa, it’s crucial to comprehend the disease’s basics.
What is Malaria?
Malaria is a life-threatening disease caused by parasites transmitted to humans through the bites of infected female Anopheles mosquitoes. Once in the human bloodstream, these parasites multiply, causing fever, headaches, and, in severe cases, complications like organ failure and death.
Malaria in Africa – A Closer Look
Malaria’s impact in Africa is particularly alarming. According to the World Health Organization (WHO), Africa accounted for 94% of all malaria cases and deaths worldwide in 2020.
Malaria Statistics in Africa
To truly grasp the gravity of malaria’s prevalence in Africa, we must examine the statistics. Malaria is the leading cause of death in Africa, especially among children under five. The WHO estimates that a child dies every two minutes from malaria in Africa, which is a sobering statistic.
Unearthing the Reasons
Several factors contribute to Africa’s high malaria rates, including ecological conditions, socioeconomic factors, and the characteristics of local malaria parasites and mosquito species.
Environmental Factors
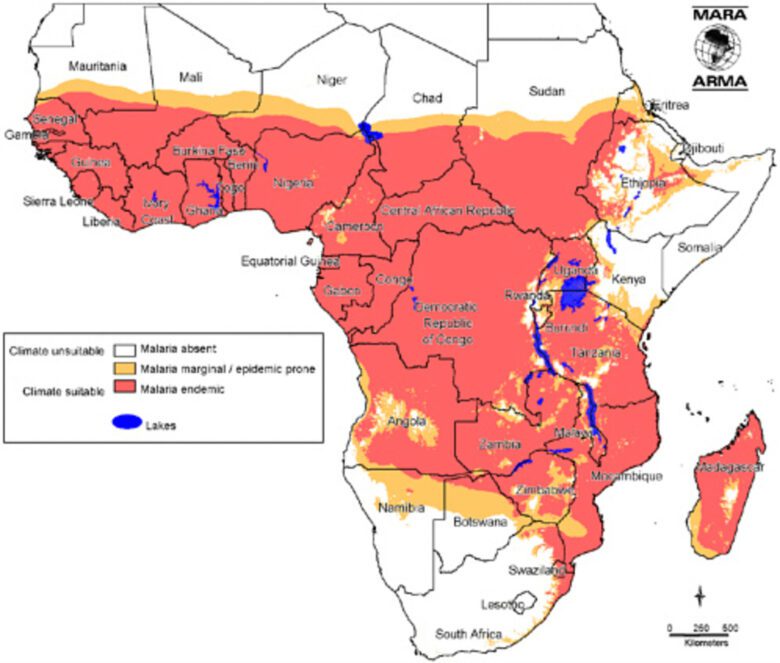
Environmental conditions in Africa provide the perfect breeding ground for Anopheles mosquitoes, the primary vectors of malaria. Warm temperatures, high humidity, and plentiful rainfall make many African regions ideal for mosquito proliferation.
Poverty plays a significant role in the malaria prevalence in Africa. Many Africans live in poorly constructed homes that offer little protection against mosquitoes. Additionally, lack of access to healthcare means many malaria cases go untreated.
Biological Factors
Africa is home to the Anopheles gambiae mosquito species, the world’s most efficient malaria vector. Additionally, the predominant malaria parasite in Africa, Plasmodium falciparum, causes the most severe form of the disease.
The Battle Against Malaria in Africa
While the fight against malaria is an uphill battle, concerted efforts are underway to combat this deadly disease.
Preventive Measures
Preventive measures include distributing insecticide-treated mosquito nets (ITNs), indoor residual spraying (IRS), and antimalarial drugs. These strategies have proven effective in reducing malaria transmission.
Research and Development
Investment in research and development is critical in the fight against malaria. The development of new tools, including more effective drugs and the first malaria vaccine, offers hope.
International Aid and Initiatives
Various international organizations and governments provide aid to Africa for malaria control. This support is crucial for funding prevention measures, treatments, and research.
The Road Ahead
While the road to eradicating malaria is long and complex, it is not impossible. By understanding why malaria is so prevalent in Africa and continuing to focus on innovative solutions, we can make strides toward a malaria-free world.
1. What is Malaria?
Malaria is a life-threatening disease caused by parasites transmitted through the bites of infected female Anopheles mosquitoes.
2. Why is Malaria more prevalent in Africa?
Several factors contribute to this, including ecological conditions, socioeconomic factors, and the biological characteristics of local malaria parasites and mosquito species.
3. What are the environmental factors contributing to Malaria in Africa?
Warm temperatures, high humidity, and plenty of rainfall make many African regions ideal breeding grounds for Anopheles mosquitoes.
4. How does poverty contribute to Malaria prevalence?
Poorly constructed homes provide little protection against mosquitoes, and lack of access to healthcare means many malaria cases go untreated.
5. Why is Anopheles gambiae significant?
Anopheles gambiae, native to Africa, is the world’s most efficient malaria vector.
6. What measures are being taken to prevent Malaria in Africa?
Preventive measures include the distribution of insecticide-treated mosquito nets, indoor residual spraying, and antimalarial drugs.
7. What role does research and development play in combating Malaria?
Research and development are crucial in creating more effective drugs, developing the first malaria vaccine, and improving prevention strategies.
8. How do international organizations help in Malaria control in Africa?
International organizations and governments provide financial aid for malaria control, funding prevention measures, treatments, and research.
9. Can Malaria be eradicated in Africa?
While the path is challenging, by understanding the reasons behind its prevalence and focusing on innovative solutions, malaria eradication is possible.
10. What is the leading cause of death in Africa?
Malaria is the leading cause of death in Africa, especially among children under five.
Conclusion
Malaria’s prevalence in Africa is a pressing issue, exacerbated by environmental, socioeconomic, and biological factors.
However, through continued research, preventive strategies, and global cooperation, there is hope for a future where malaria no longer disproportionately affects Africa.