Health
The Shocking Truth about Malaria and Poverty

The Shocking Truth about Malaria and Poverty
Malaria is a disease that affects millions of people worldwide, with the majority of cases being in sub-Saharan Africa.
The disease is caused by the Plasmodium parasite, which is transmitted through the bites of infected female Anopheles mosquitoes.
Malaria can cause severe symptoms such as fever, chills, and headache, and can even be fatal if left untreated.
But what many people don’t realize is the strong connection between malaria and poverty.
In this article, we will explore the shocking truth about malaria and poverty, including the impact of malaria on
the economy, the social cost of the disease, and efforts to combat malaria in impoverished areas.
Understanding Malaria
What is Malaria?
Malaria is a disease caused by the Plasmodium parasite.
The parasite is transmitted through the bites of infected female Anopheles mosquitoes.
There are four different types of Plasmodium parasites that can cause malaria in humans:
Plasmodium falciparum, Plasmodium vivax, Plasmodium ovale, and Plasmodium malariae.
Malaria is most prevalent in sub-Saharan Africa, where it is a leading cause of death.
Malaria is a life-threatening disease caused by the Plasmodium parasite, which is transmitted to humans through the bites of infected female Anopheles mosquitoes.
The disease is most prevalent in tropical and subtropical regions, particularly in sub-Saharan Africa, but also in Asia and South America.
Once the Plasmodium parasite enters the human body, it travels to the liver where it multiplies and infects red blood cells.
This causes a range of symptoms including fever, chills, headache, muscle aches, and fatigue.
In severe cases, malaria can cause anemia, seizures, kidney failure, and even death.
There are five species of Plasmodium that cause malaria in humans, with Plasmodium falciparum being the most deadly.
It is responsible for the majority of malaria-related deaths, especially in young children and pregnant women.
Other species such as Plasmodium vivax, Plasmodium ovale, Plasmodium malaria, and Plasmodium knowlesi
are also found in humans and cause milder forms of malaria.
Malaria can be prevented through several means, including using insecticide-treated mosquito nets,
spraying insecticides in homes, and taking antimalarial medications.
The World Health Organization (WHO) recommends the use of artemisinin-based combination therapies
(ACTs) to treat uncomplicated malaria caused by Plasmodium falciparum, while other forms of malaria can be
treated with other antimalarial medications.
Efforts to combat malaria have been ongoing for many years, with significant progress made in reducing the
a number of cases and deaths.
However, the disease remains a major global health problem, with an estimated 229 million cases and
409,000 deaths worldwide in 2019, according to the WHO.
Continued investment in prevention, treatment, and research is necessary to achieve the goal of eradicating malaria.
Signs and Symptoms of Malaria The symptoms of malaria can vary from mild to severe and can include fever,
chills, headache, muscle pain, and fatigue.
In severe cases, malaria can cause anemia, respiratory distress, and organ failure.
Malaria can also cause complications in pregnant women, including premature delivery and low birth weight.
Malaria Prevention Malaria prevention involves a combination of measures, including the use of insecticides-
treated bed nets, indoor residual spraying, and antimalarial drugs.
Insecticide-treated bed nets are particularly effective at preventing malaria transmission, as they create a
a physical barrier between humans and infected mosquitoes.
Indoor residual spraying involves the application of insecticides to the walls and surfaces of homes to kill
mosquitoes.
Antimalarial drugs are used to treat and prevent malaria and include drugs such as chloroquine, artemisinin-
based combination therapies, and mefloquine.
The Economic Impact of Malaria
Malaria and Poverty Malaria is both a cause and a consequence of poverty.
The disease disproportionately affects the poor, who are more likely to live in areas with poor sanitation and inadequate healthcare.
Malaria can also lead to poverty by causing lost productivity, increased healthcare costs, and decreased economic growth.
Malaria is a life-threatening disease caused by the Plasmodium parasite, which is transmitted through the
bites of infected female Anopheles mosquitoes.
While it is a significant public health challenge, malaria also has a considerable economic impact, particularly
in developing countries where it is most prevalent.
Firstly, malaria has a significant economic impact on individuals and households.
People who contract malaria often experience symptoms such as fever, chills, and fatigue, which can prevent
them from working, leading to lost income.
Additionally, the cost of treatment, including medication and hospitalization, can be substantial, pushing
affected households into poverty.
In many cases, families may need to sell assets, take on debt, or use savings to cover medical expenses.
Secondly, malaria has a broader impact on the economy of the affected regions.
The disease can reduce productivity by keeping workers away from their jobs, leading to a decrease in
economic output.
This can impact both small businesses and large industries, particularly those that rely on manual labor.
Moreover, malaria affects the tourism industry, as the disease is often associated with countries with high
infection rates, leading to a drop in tourism revenues.
Thirdly, the cost of controlling and preventing malaria can be substantial for governments.
Funds allocated for malaria control and treatment could be redirected to other public health programs or
initiatives if malaria did not exist.
The cost of controlling malaria through measures such as insecticide-treated bed nets, indoor residual
spraying, and anti-malarial drugs can be a considerable financial burden, particularly for resource-limited countries.
Lastly, malaria can also impact international trade and investment.
Countries with high malaria rates may be perceived as risky by potential investors, making it difficult to
attract foreign investment.
Additionally, restrictions on travel and trade may be imposed due to fears of the disease spreading, causing
disruptions to global supply chains.
The Cost of Malaria Malaria has a high economic cost, both in terms of direct medical expenses and lost productivity.
In sub-Saharan Africa, where the disease is most prevalent, malaria is estimated to cost the economy $12 billion per year.
This includes the cost of treatment, lost productivity due to illness, and decreased economic growth
Malaria and Education Malaria can also have an impact on education.
Children who contract malaria are more likely to miss school due to illness, which can lead to decreased
educational achievement.
In addition, families may be forced to spend money on healthcare costs for malaria treatment instead of
education expenses.
The Social Impact of Malaria
Malaria and Social Inequality Malaria is a disease that disproportionately affects the poor, who are more likely
to live in areas with inadequate healthcare and poor sanitation.
This creates a cycle of poverty and illness, where malaria perpetuates social inequality.
Malaria is a disease caused by a parasite that is transmitted to humans through the bites of infected mosquitoes.
Despite being a preventable and treatable disease, malaria still causes significant social impact, particularly in developing countries.
Here are some shocking truths about the social impact of malaria:
- Malaria is a major cause of mortality: According to the World Health Organization (WHO), there were 229 million cases of malaria worldwide in 2019, leading to 409,000 deaths.
- The majority of deaths were in sub-Saharan Africa, where the disease disproportionately affects children under the age of five.
- Malaria is a barrier to economic development: Malaria is responsible for an estimated loss of 1.3% of economic growth per year in endemic countries.
- The disease can cause individuals to miss work and school, leading to decreased productivity and income.
- It also places a burden on healthcare systems, diverting resources that could be used for other health issues.
- Malaria perpetuates poverty: Malaria is both a cause and consequence of poverty. Poor living conditions, inadequate healthcare, and lack of access to prevention and treatment contribute to the disease’s prevalence in poor communities.
- Additionally, the cost of malaria treatment and lost income due to illness can push families further into poverty.
- Malaria disproportionately affects vulnerable populations: Malaria affects those who are already marginalized the most.
- Pregnant women, children, and individuals with HIV/AIDS are particularly vulnerable to the disease’s severe effects.
- Malaria is preventable and treatable: The use of insecticide-treated bed nets, indoor residual spraying, and timely diagnosis and treatment can significantly reduce the incidence of malaria. many people living in endemic countries lack access to these tools, resulting in preventable deaths and illnesses.
The social impact of malaria is significant, affecting individuals, families, and entire communities.
Addressing the disease’s root causes and improving access to prevention and treatment is crucial to
reducing the disease’s impact on vulnerable populations.
Malaria and Gender Inequality Malaria can also have an impact on gender inequality.
Women and girls are more likely to contract malaria due to their increased exposure to mosquitoes, and they
may also experience more severe symptoms of the disease.
In addition, the burden of caring for family members with malaria often falls on
In conclusion
malaria has significant economic consequences on individuals, households, industries, and governments in the affected regions.
Its impact extends beyond health outcomes and requires concerted efforts from various stakeholders to mitigate its adverse economic effects.
Health
6 Daily Habits to Naturally Lower Cholesterol Levels
Health
Understanding the Rapid Spread of Monkeypox’s New Strain Clade 1b
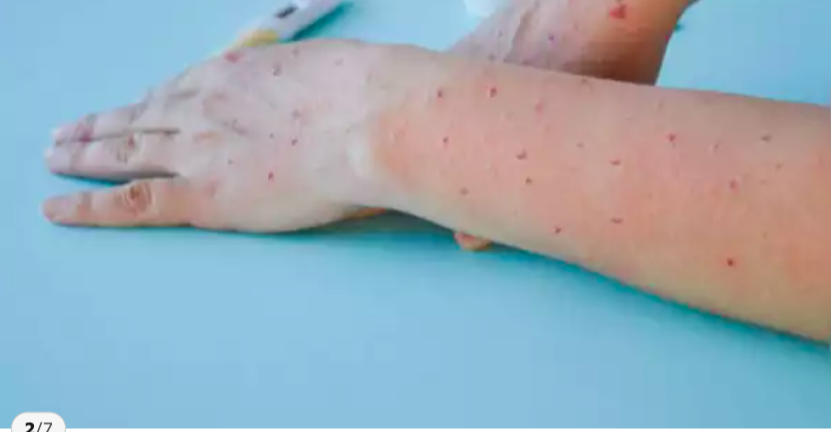
Understanding the Rapid Spread of Monkeypox’s New Strain Clade 1b: Key Facts on Transmission, Symptoms, Severity, and Vaccination
Monkeypox, a viral disease with symptoms resembling smallpox, has recently gained attention due to the emergence of a newstrain, Clade 1b.
This article delves into the essential details about this new variant, including how it spreads, its symptoms, its severity, and the current state of vaccinations.
Our goal is to provide a comprehensive and clear understanding of this evolving situation, enabling readers to stay informed and prepared.
Monkeypox, once a rare and somewhat obscure disease, has recently become a significant public health concern due to the emergence of new strains.
Among these, Clade 1b has been noted for its rapid spread and distinct characteristics.
As we navigate through the complexities of this variant, it is crucial to grasp the fundamentals of its transmission, symptoms, severity, and preventive measures, including vaccination.
Understanding Monkeypox Clade 1b
What is Monkeypox?
Monkeypox is a zoonotic virus belonging to the Orthopoxvirus genus, which also includes smallpox.
First identified in monkeys, it can infect humans through close contact with infected animals or individuals.
While it shares similarities with smallpox, monkeypox tends to be less severe and less transmissible.
Clade 1b Overview
Monkeypox has several clades (strains), with Clade 1b being the most recent and notable for its rapid spread.
This strain has shown increased transmissibility compared to previous clades, raising concerns among public health officials.
Transmission of Clade 1b
Modes of Transmission
Clade 1b spreads primarily through:
- Direct Contact: Contact with bodily fluids, skin lesions, or contaminated surfaces of an infected person.
- Respiratory Droplets: Prolonged face-to-face interaction can lead to transmission through respiratory droplets.
- Animal Contact: Infected animals, particularly rodents and primates, can transmit the virus to humans.
Environmental Factors
Transmission rates can also be influenced by environmental factors such as:
- Crowded Living Conditions: Higher transmission rates are observed in densely populated areas.
- Sanitation Practices: Poor hygiene and sanitation can facilitate the spread of the virus.
Symptoms of Monkeypox Clade 1b
Early Symptoms
The symptoms of Clade 1b may resemble those of other viral infections, making initial diagnosis challenging.
Early symptoms include:
- Fever: A sudden onset of high temperature.
- Headache: Severe headaches that can persist for days.
- Muscle Aches: Generalized muscle pain and discomfort.
- Fatigue: Extreme tiredness and weakness.
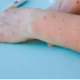
Rash and Skin Lesions
A defining feature of monkeypox is the rash, which typically progresses through several stages:
- Macules: Flat, discolored spots on the skin.
- Papules: Raised bumps.
- Vesicles: Fluid-filled blisters.
- Pustules: Pus-filled lesions that eventually crust over.
Severe Symptoms
In more severe cases, symptoms may include:
- Encephalitis: Inflammation of the brain, leading to neurological symptoms.
- Pneumonia: Infection of the lungs that can cause difficulty breathing.
- Secondary Infections: Bacterial infections that may complicate the healing process.
Severity of Clade 1b
General Outlook
Clade 1b has been associated with a higher transmission rate and more severe outcomes compared to other strains. However, the overall severity can vary widely among individuals.
Factors influencing severity include:
- Immune System Status: Individuals with weakened immune systems or pre-existing conditions may experience more severe symptoms.
- Age: Young children and elderly individuals are at higher risk of severe illness.
- Timeliness of Medical Care: Early medical intervention can significantly affect the outcome.
Mortality Rates
The mortality rate for Clade 1b is currently under study, but initial data suggest it may be higher than previous strains. Prompt medical attention and supportive care are crucial in reducing the risk of severe outcomes.
Vaccination and Prevention
Current Vaccines
Vaccination is a key strategy in controlling the spread of monkeypox.
The following vaccines are relevant:
- Smallpox Vaccine: The smallpox vaccine is effective against monkeypox due to the similarities between the viruses. It provides protection for those who have been recently vaccinated or who received it in the past.
- Monkeypox-Specific Vaccine: Research is ongoing into vaccines specifically targeting monkeypox, with several candidates showing promise in trials.
Vaccination Recommendations
Public health authorities recommend vaccination for:
- Healthcare Workers: Individuals who are at higher risk due to their profession.
- High-Risk Populations: People in areas experiencing outbreaks or those with frequent exposure to infected individuals.
Preventive Measures
In addition to vaccination, preventive measures include:
- Good Hygiene: Regular handwashing and use of hand sanitizers.
- Avoiding Contact: Minimizing close contact with individuals displaying symptoms or with infected animals.
- Isolation: Infected individuals should isolate themselves to prevent the spread of the virus.
Conclusion
The emergence of Monkeypox Clade 1b represents a significant challenge to global health. Its increased transmissibility and potential for severe outcomes highlight the importance of staying informed and proactive.
By understanding its transmission, symptoms, and preventive measures, individuals and communities can better protect themselves and mitigate the impact of this new strain.
FAQs
1. What makes Clade 1b different from other monkeypox strains?
Clade 1b is noted for its increased transmissibility and potentially more severe outcomes compared to other strains.
It spreads faster and may lead to more serious health issues, necessitating closer monitoring and enhanced preventive measures.
2. How can I tell if I have monkeypox or another viral infection?
Monkeypox often begins with flu-like symptoms and progresses to a distinct rash.
If you experience these symptoms, especially if you’ve been in contact with someone who has monkeypox or are in an outbreak area, seek medical advice for accurate diagnosis and testing.
3. Is the smallpox vaccine effective against Monkeypox Clade 1b?
Yes, the smallpox vaccine offers protection against monkeypox, including Clade 1b, due to the similarities between the two viruses.
However, its effectiveness may vary based on factors such as time since vaccination and individual health conditions.
4. Are there any new vaccines specifically for monkeypox?
Research is ongoing to develop and approve vaccines specifically targeting monkeypox.
Several candidates are in various stages of clinical trials, with some showing promising results in enhancing protection against monkeypox strains, including Clade 1b.
5. What should I do if I suspect I have monkeypox?
If you suspect you have monkeypox, contact a healthcare provider immediately. They can guide you through testing, diagnosis, and appropriate care.
In the meantime, practice good hygiene and avoid close contact with others to prevent spreading the virus.
References:
Health
Understanding the Low Risk of Mpox Outbreak in India and Our Preparedness Measures

-

 Trending Stories1 year ago
Trending Stories1 year agoCDC: 1 in 4 Americans Still COVID-Free by End of 2022
-

 Health5 years ago
Health5 years agoMeghan Trainor Shares Motivational New Song ‘Blink’
-

 Health2 years ago
Health2 years agoHow Long Does Monkey Pox Last Before It Surfaces in the Body?
-

 Health2 years ago
Health2 years agoWhat Causes Swollen Body? Understanding Edema and its Triggers
-

 Health4 months ago
Health4 months agoHow Do Pawpaw Seeds Support Cardiovascular Health?
-

 Health3 years ago
Health3 years agoNutrition and the Importance of a Fitness Program – 3 Things to Know
-

 Health3 years ago
Health3 years ago5 Weird Reasons Why Pimples Disappear After Marriage
-

 Health2 years ago
Health2 years agoHealth Benefits Of Pawpaw Seed? 7 Things To Know