Health
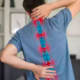
The Causes of Pain on the Left Side of the Abdomen

Last Updated on July 18, 2023 by Nurse Vicky
Unraveling the Mystery: The Causes of Pain on the Left Side of the Abdomen
Abdominal pain can be an unsettling experience, and when it occurs on the left side, it often leaves us in a quandary. The pain can be sharp and sudden or dull and constant. Either way, the question arises: what could be the underlying cause?
Understanding Your Abdomen
To begin our exploration, it’s important to understand the structure of the abdomen. On the left side, several organs come into play: the stomach, the left kidney, part of the liver, the spleen, portions of the pancreas and large intestine, and in women, the left ovary and fallopian tube.
Any disease or injury to these organs can manifest as pain on the left side of the abdomen. Let’s delve deeper into the common conditions that could be the culprit.
Gastric Causes
Gastritis and Gastric Ulcers
The stomach, being the main organ on the left side of the abdomen, is often the source of left-sided abdominal pain. Gastritis, an inflammation of the stomach lining, often results in dull pain. It can be caused by factors like excessive alcohol consumption, long-term use of certain medications, bacterial infections, and diseases like Crohn’s and autoimmune disorders.
Gastric ulcers, on the other hand, are painful sores on the stomach lining. They usually cause a burning sensation or pain in the middle or left side of the abdomen, especially on an empty stomach.
Gastroenteritis
Commonly known as a stomach bug, gastroenteritis is characterized by inflammation of the gastrointestinal tract, including the stomach and intestines. It is usually caused by a bacterial or viral infection. Symptoms can include left-sided abdominal pain, diarrhea, vomiting, and dehydration.
Pancreatic Causes
The pancreas, though predominantly located on the left side of the abdomen, can cause pain on either side or even radiate to the back.
Pancreatitis refers to inflammation of the pancreas, which can be acute or chronic. Acute pancreatitis often presents as severe, sudden pain in the abdomen, whereas chronic pancreatitis manifests as recurring or persistent abdominal pain.
Splenic Causes
Splenomegaly
The spleen, located on the upper left side of the abdomen, generally doesn’t cause pain unless it becomes enlarged—a condition called splenomegaly.
This enlargement could be due to various reasons such as infection, liver diseases, blood diseases, or cancer. Symptoms are usually vague but can include pain or fullness in the left upper abdomen that may spread to the left shoulder.
Renal Causes
Kidney Stones
The left kidney, located towards the back of the abdomen, can cause pain when there is an issue, such as a kidney stone. This solid mass forms from crystals in the urine and can cause severe pain in the back or side, beneath the ribs, or the lower abdomen and groin. The pain often comes in waves and fluctuates in intensity.
Kidney Infection
A kidney infection, or pyelonephritis, often causes severe, one-sided back pain that can extend to the lower abdomen. Other symptoms can include fever, frequent urination, and blood or pus in the urine.
Gynecological Causes (in Women)
Ovarian Cysts
In women, left-sided abdominal pain can originate from the reproductive system. One common cause is ovarian cysts. These fluid-filled sacs form on the ovaries and are often painless. However, if a cyst ruptures or causes the ovary to twist, it can cause sudden, severe pain on one side of the lower abdomen, including the left side.
Ectopic Pregnancy
An ectopic pregnancy, where a fertilized egg implants outside the uterus, can also cause lower left abdominal pain. This is a medical emergency and needs immediate attention.
Digestive Tract Causes
Diverticulitis, an inflammation or infection of small pouches that can form in the wall of the colon, can cause persistent pain in the lower left abdomen, fever, and constipation or diarrhea.
Inflammatory Bowel Disease (IBD)
Conditions such as Crohn’s disease and ulcerative colitis, part of a group of disorders known as IBD, can cause long-term inflammation and sores in the digestive tract, leading to symptoms like abdominal pain, cramping, and diarrhea.
When to Seek Medical Help
Understanding the potential causes of left-sided abdominal pain can help you identify the severity of your condition. However, it’s crucial to seek immediate medical attention if your abdominal pain is severe, lasts more than a few hours, or is accompanied by other symptoms like fever, nausea, vomiting, unexplained weight loss, or yellowing of the skin and eyes.
Frequently Asked Questions
What could be the cause of sharp pain on the left side of the abdomen?
Sharp pain on the left side of the abdomen could be due to conditions like kidney stones, diverticulitis, or in women, ovarian cysts or ectopic pregnancy.
Can gas cause pain on the left side of the abdomen?
Yes, gas can cause pain on either side of the abdomen due to the accumulation of gas in the digestive tract.
Is pain on the left side of the abdomen a sign of a heart attack?
While heart attacks typically cause chest pain, they can sometimes present as upper abdominal pain, nausea, or indigestion. However, this pain is usually central or on the right side, not typically on the left side.
Can stress cause left-sided abdominal pain?
Yes, stress can cause a variety of physical symptoms, including abdominal pain. This is due to the body’s response to stress, which can include slowed digestion and tightened stomach muscles.
Can left-sided abdominal pain be a sign of cancer?
Certain types of cancer, like stomach, colon, and ovarian cancer, can cause left-sided abdominal pain. However, pain alone is a non-specific symptom and usually accompanies other symptoms like unexplained weight loss and changes in bowel habits.
How is the cause of left-sided abdominal pain diagnosed?
Diagnosis usually involves a combination of a physical examination, medical history, and tests like blood tests, urine tests, imaging studies (like X-rays, CT scans, or ultrasounds), and endoscopic procedures.
Is left-sided abdominal pain always a cause for concern?
Not always. While it can be a sign of various medical conditions, some causes, like gas or indigestion, are not serious. However, severe, persistent, or worsening pain should always be evaluated by a doctor.
What home remedies can help with left-sided abdominal pain?
Home remedies depend on the cause of the pain. Over-the-counter antacids could help with indigestion. A heating pad could ease muscle tension or menstrual cramps.
For gas, over-the-counter gas relief medications or dietary changes can help. It’s important to note that these remedies should not replace medical advice, especially for severe or persistent pain.
What kind of doctor should I see for left-sided abdominal pain?
A primary care physician should be the first point of contact. Depending on the suspected cause, you may be referred to a gastroenterologist (for digestive tract issues), a urologist (for kidney issues), or a gynecologist (for women’s reproductive issues).
Can drinking water help with left-sided abdominal pain?
Staying hydrated can help with certain causes of abdominal pain, like kidney stones and constipation. However, it won’t cure underlying conditions, and it’s important to seek medical advice for ongoing or severe pain.
Conclusion
Pain in the left side of the abdomen can be attributed to various causes, ranging from gastric issues to kidney stones to gynecological problems in women.
By understanding the possible causes, you can better communicate your symptoms to your healthcare provider, leading to faster diagnosis and effective treatment. Remember, timely medical advice is key when dealing with abdominal pain.
References and Further Reading
- Gastritis – Symptoms and causes – Mayo Clinic
- Gastroenteritis – Symptoms and causes – Mayo Clinic
- Pancreatitis – Symptoms and causes – Mayo Clinic
- Kidney stones – Symptoms and causes – Mayo Clinic
- Ovarian cysts – Symptoms and causes – Mayo Clinic
- Ectopic pregnancy – Symptoms and causes – Mayo Clinic
- Diverticulitis – Symptoms and causes – Mayo Clinic
- Crohn’s disease – Symptoms and causes – Mayo Clinic
Health
Hair Gummies: A Trend Worth Your Time or Just Another Health Fad?

Hair Gummies: A Trend Worth Your Time or Just Another Health Fad?
In recent years, hair gummies have taken the health and beauty world by storm, boasting promises of luscious locks and a speedy route to hair health.
But with an array of products flooding the market, it’s essential to separate fact from fiction.
Are these colorful, chewy supplements a miracle solution for your hair troubles, or are they simply a trendy snack with little efficacy?
In this comprehensive article, we will explore the science behind hair gummies, their ingredients, potential benefits, and the questions surrounding their effectiveness.
Understanding Hair Health
The Basics of Hair Growth
To fully grasp the impact of hair gummies, it’s vital to understand how hair grows.
Each strand of hair goes through three main phases:
- Anagen Phase: This is the active growth phase, which can last several years. The length of this phase varies among individuals.
- Catagen Phase: A transitional phase lasting a few weeks, where hair growth slows, and the hair follicle shrinks.
- Telogen Phase: The resting phase, lasting a few months before the hair falls out, making way for new growth.
Hair health is influenced by a variety of factors, including genetics, hormones, diet, and overall health.
As such, a balanced approach to hair care, encompassing nutrition, proper hair care routines, and avoiding damaging practices, is essential.
Common Causes of Hair Issues
Hair loss or poor hair health can arise from numerous factors:
- Nutritional Deficiencies: A lack of essential vitamins and minerals can hinder hair growth.
- Hormonal Changes: Conditions like pregnancy, menopause, and thyroid disorders can significantly affect hair health.
- Stress: Chronic stress can trigger hair loss through a condition known as telogen effluvium.
- Medical Conditions: Certain diseases and medications can also contribute to hair loss.
What Are Hair Gummies?
Hair gummies are dietary supplements designed to promote hair health.
They are usually made with a combination of vitamins, minerals, and sometimes botanical extracts, often marketed as a convenient and tasty alternative to traditional vitamin pills.
Key Ingredients in Hair Gummies
While formulations vary, here are some common ingredients found in hair gummies:
- Biotin: A B-vitamin known for its role in hair and nail health. Biotin deficiencies can lead to brittle hair and hair loss.
- Vitamins A, C, and E: Antioxidants that help protect hair from oxidative stress, promoting a healthy scalp and hair growth.
- Folic Acid: Important for cell growth and regeneration, folic acid is believed to support healthy hair follicles.
- Zinc: Plays a role in hair tissue growth and repair, making it a crucial mineral for maintaining healthy hair.
- Collagen: An essential protein for skin elasticity that may also benefit hair strength and growth.
Do Hair Gummies Really Work?
The Science Behind Hair Gummies
While the ingredients in hair gummies are known to contribute to hair health, the question remains:
Do they work as effectively as claimed?
Here’s what the research suggests:
- Biotin: Studies have shown that biotin can improve hair thickness in those with deficiencies, but most people get sufficient biotin from their diet. Supplementing with biotin may not yield significant benefits for individuals who are not deficient.
- Vitamins and Minerals: Research indicates that vitamins A, C, D, E, and minerals like zinc and iron play a role in maintaining healthy hair. However, simply taking these vitamins in gummy form doesn’t guarantee results unless there’s a deficiency present.
- Collagen: Some studies suggest that collagen supplements can improve hair and skin health by providing amino acids essential for protein synthesis. However, more research is needed to establish direct benefits for hair growth.
User Experiences and Anecdotes
While anecdotal evidence often highlights positive experiences with hair gummies, it’s important to approach these testimonials with caution. Individual results may vary, and factors such as diet, overall health, and genetics play significant roles in hair health.
Potential Benefits of Hair Gummies
While not a miracle solution, hair gummies may offer certain benefits:
- Convenient Form: For those who struggle with swallowing pills, gummies provide a palatable alternative.
- Added Nutrients: If you have a deficiency in specific vitamins or minerals, hair gummies can supplement your diet effectively.
- Increased Awareness of Nutrition: Taking supplements can prompt individuals to pay more attention to their overall nutritional intake.
- Improved Hair Appearance: Users may notice shinier and healthier-looking hair due to the vitamins and antioxidants present in these products.
Are There Risks?
While hair gummies are generally safe, there are some considerations to keep in mind:
- Overconsumption: Gummies are often flavored and sweetened, which may lead to overconsumption and potential digestive issues.
- Sugar Content: Many gummies contain added sugars, which can contribute to other health problems if consumed excessively.
- Interactions with Other Supplements: If you’re taking other vitamins or supplements, it’s essential to ensure you’re not exceeding recommended doses, particularly for fat-soluble vitamins like A and E, which can accumulate in the body.
What Experts Say
Dermatologists and nutritionists often emphasize a balanced diet over reliance on supplements.
They suggest that whole foods—rich in vitamins, minerals, and healthy fats—are the best source for hair health.
Foods such as leafy greens, nuts, seeds, fish, and eggs can provide essential nutrients without the added sugars and potential downsides of gummies.
Conclusion:
Fad or Fact?
In conclusion, hair gummies may not be the ultimate solution for hair health, but they can serve as a helpful supplement for those with specific nutritional deficiencies.
They are convenient and may improve the overall appearance of hair for some users. However, it’s crucial to approach them with realistic expectations and prioritize a balanced diet rich in whole foods.
If you’re considering adding hair gummies to your routine, consult with a healthcare provider or nutritionist to ensure you’re making an informed decision that aligns with your health goals.
FAQs
1. Can hair gummies replace a balanced diet?
No, hair gummies are supplements and should not replace a balanced diet. They can help fill nutritional gaps but should be taken alongside a healthy eating plan.
2. How long does it take to see results from hair gummies?
Results vary, but users may start noticing improvements in hair texture and appearance after 4-12 weeks of consistent use.
3. Are hair gummies safe for everyone?
Most hair gummies are safe for general use; however, individuals with specific health conditions or allergies should consult a healthcare professional before taking them.
4. Can I take hair gummies with other supplements?
Yes, but be cautious of total vitamin and mineral intake to avoid exceeding recommended daily allowances. Consult with a healthcare provider for personalized advice.
5. Are there any side effects of hair gummies?
Some users may experience digestive issues, allergic reactions, or headaches due to high sugar content or specific ingredients. It’s best to start with a small dose to assess tolerance.
References:
Health
Understanding the Spine: Common Conditions and Effective Solutions
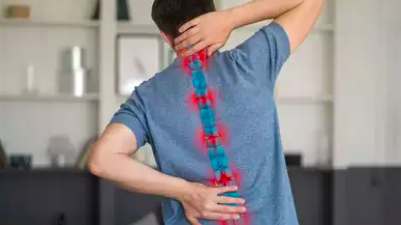
Understanding the Spine: Common Conditions and Effective Solutions
The spine is an essential structure in the human body, acting as a central pillar that supports our posture, facilitates movement, and protects the spinal cord.
Despite its importance, many individuals experience various spine-related conditions that can impact their quality of life.
In this comprehensive article, we will explore common spinal conditions, their causes, symptoms, and effective methods to address them.
What is the Spine?
The spine, also known as the vertebral column, is composed of 33 vertebrae arranged in a flexible yet sturdy structure.
It serves several critical functions:
- Support: The spine supports the head and allows for an upright posture.
- Protection: It encases and protects the spinal cord, a crucial component of the central nervous system.
- Mobility: The spine allows for a wide range of movements, including bending, twisting, and turning.
- Weight Distribution: It helps distribute weight and absorbs shock during activities like walking or running.
Understanding the structure and function of the spine is vital for recognizing and addressing the conditions that can affect it.
Common Spinal Conditions
Several conditions can adversely impact the spine, leading to pain, discomfort, and reduced mobility. Here are some of the most common spinal conditions:
1. Herniated Discs
A herniated disc occurs when the soft inner material of a spinal disc bulges out through a tear in the outer layer. This can compress nearby nerves, leading to pain, numbness, or weakness in the arms or legs.
Causes:
- Age-related degeneration
- Heavy lifting or sudden movements
- Trauma or injury
Symptoms:
- Localized back pain
- Radiating pain to the limbs
- Numbness or tingling
Treatment:
- Physical therapy
- Pain management through medications
- In severe cases, surgery may be required.
2. Spinal Stenosis
Spinal stenosis is the narrowing of the spinal canal, which can lead to pressure on the spinal cord and nerves. This condition often occurs in the cervical (neck) or lumbar (lower back) regions.
Causes:
- Age-related changes in the spine
- Osteoarthritis
- Herniated discs
Symptoms:
- Pain or cramping in the legs
- Weakness or numbness
- Difficulty walking or standing for extended periods
Treatment:
- Physical therapy and exercise
- Medications for pain relief
- In some cases, surgical decompression may be necessary.
3. Scoliosis
Scoliosis is an abnormal curvature of the spine, often appearing in childhood or adolescence. While many cases are mild, severe scoliosis can lead to complications.
Causes:
- Idiopathic (unknown cause)
- Congenital (present at birth)
- Neuromuscular conditions
Symptoms:
- Uneven shoulders or hips
- Visible curvature of the spine
- Back pain
Treatment:
- Monitoring and observation for mild cases
- Bracing for growing children
- Surgery for severe curvatures.
4. Osteoporosis
Osteoporosis is a condition characterized by weakened bones, making them more susceptible to fractures. This is particularly concerning for the vertebrae, which can lead to compression fractures.
Causes:
- Aging
- Hormonal changes
- Lack of calcium and vitamin D
Symptoms:
- Height loss
- Back pain due to fractures
- A stooped posture
Treatment:
- Medications to strengthen bones
- Nutritional supplements (calcium and vitamin D)
- Weight-bearing exercises to improve bone density.
5. Degenerative Disc Disease
Degenerative disc disease refers to the wear and tear of spinal discs over time, leading to pain and reduced flexibility.
Causes:
- Age-related degeneration
- Repetitive stress on the spine
- Genetics
Symptoms:
- Chronic back pain
- Pain that worsens with movement
- Possible radiating pain in the limbs
Treatment:
- Physical therapy and exercise
- Pain management strategies
- Surgical options for severe cases.
Preventing Spinal Conditions
While some spinal conditions are unavoidable due to genetics or aging, many can be prevented or mitigated through healthy lifestyle choices.
Here are some preventative measures:
1. Maintain Good Posture
Proper posture helps reduce strain on the spine. When sitting, keep your back straight, shoulders relaxed, and feet flat on the ground. When standing, distribute your weight evenly on both feet.
2. Stay Active
Regular physical activity strengthens the muscles that support the spine and improves flexibility. Aim for a balanced routine that includes strength training, aerobic exercise, and stretching.
3. Ergonomic Work Environment
If you spend long hours at a desk, ensure your workspace is ergonomically designed. Adjust your chair, desk height, and computer monitor to reduce strain on your back and neck.
4. Healthy Weight Management
Maintaining a healthy weight reduces stress on the spine and helps prevent conditions like degenerative disc disease and spinal stenosis.
5. Avoid Smoking
Smoking impairs blood flow and can lead to spinal degeneration. Quitting smoking can improve overall health and reduce the risk of spinal issues.
Effective Treatments for Spinal Conditions
If you experience spine-related pain or discomfort, it’s essential to consult a healthcare professional for a proper diagnosis and treatment plan.
Here are some common treatment options:
1. Physical Therapy
Physical therapists develop personalized exercise programs to strengthen the back muscles, improve flexibility, and alleviate pain. They may also use techniques like ultrasound or electrical stimulation to manage discomfort.
2. Medications
Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can help manage mild to moderate pain. Prescription medications may be necessary for more severe pain or inflammation.
3. Injections
Corticosteroid injections can reduce inflammation and provide temporary relief for conditions like herniated discs or spinal stenosis. These are typically used when other treatments have failed.
4. Surgery
In severe cases, surgery may be necessary to relieve pressure on the spinal cord or nerves. Common surgical procedures include discectomy (removal of herniated disc material), spinal fusion, and laminectomy (removal of part of the vertebra).
5. Alternative Therapies
Complementary treatments like acupuncture, chiropractic care, and massage therapy may provide relief for some individuals. Always consult with a healthcare professional before trying alternative therapies.
Conclusion
Understanding the spine and its common conditions is crucial for maintaining a healthy lifestyle and preventing potential issues.
By recognizing symptoms early and seeking appropriate treatment, individuals can address spinal conditions effectively.
Implementing preventative measures, such as maintaining good posture and staying active, can significantly reduce the risk of developing spine-related issues.
Prioritize your spinal health, consult with professionals when necessary, and take proactive steps to ensure a healthy and pain-free back.
FAQs
1. What are the common symptoms of spinal conditions?
Common symptoms include localized back pain, radiating pain in the limbs, numbness, tingling sensations, and difficulty with movement.
2. How can I improve my posture while working?
To improve your posture at work, adjust your chair and desk height, use a supportive chair, and ensure your computer screen is at eye level.
3. Can physical therapy help with spinal conditions?
Yes, physical therapy can help strengthen back muscles, improve flexibility, and alleviate pain associated with various spinal conditions.
4. When should I see a doctor for back pain?
If you experience persistent back pain that does not improve with rest, is accompanied by numbness or weakness, or interferes with daily activities, it’s essential to see a doctor.
5. Are there lifestyle changes I can make to prevent spinal issues?
Yes, maintaining a healthy weight, staying active, practicing good posture, and avoiding smoking can help prevent spinal conditions.
References:
Health
Understanding the Causes of Premature Menopause in Women
-

 Trending Stories1 year ago
Trending Stories1 year agoCDC: 1 in 4 Americans Still COVID-Free by End of 2022
-

 Health5 years ago
Health5 years agoMeghan Trainor Shares Motivational New Song ‘Blink’
-

 Health6 months ago
Health6 months agoHow Do Pawpaw Seeds Support Cardiovascular Health?
-

 Health2 years ago
Health2 years agoHow Long Does Monkey Pox Last Before It Surfaces in the Body?
-

 Health3 years ago
Health3 years agoWhat Causes Swollen Body? Understanding Edema and its Triggers
-

 Health3 years ago
Health3 years agoNutrition and the Importance of a Fitness Program – 3 Things to Know
-

 Health3 years ago
Health3 years ago5 Weird Reasons Why Pimples Disappear After Marriage
-

 Health2 years ago
Health2 years agoHealth Benefits Of Pawpaw Seed? 7 Things To Know