Health
Unraveling the Mystery: What Is the Main Cause of Leg Ulcers?
Last Updated on May 20, 2023 by Nurse Vicky
Unraveling the Mystery: What Is the Main Cause of Leg Ulcers?
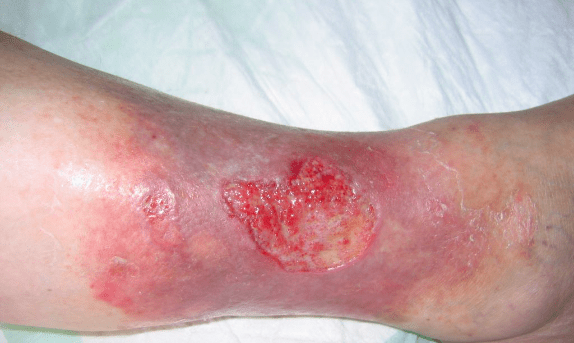
Leg ulcers are a common and often distressing condition that affects millions of people worldwide. These open sores on the lower leg can be painful, slow to heal, and significantly impact a person’s quality of life. Understanding the main cause of leg ulcers is crucial for effective treatment and prevention.
In this comprehensive article, we will delve into the intricacies of leg ulcers, explore their primary causes, and provide valuable insights to help you better manage this condition. So, let’s unravel the mystery and gain a deeper understanding of what lies behind leg ulcers.
What are Leg Ulcers?
Leg ulcers are open sores or wounds that develop on the lower leg, typically below the knee and above the ankle. These ulcers can be shallow or deep and may take a long time to heal. They often result from underlying medical conditions and are associated with impaired blood circulation, especially in the veins and arteries of the legs.
Understanding the Circulatory System and Its Role
To comprehend the causes of leg ulcers, it’s essential to have a basic understanding of the circulatory system. The circulatory system comprises the heart, blood vessels, and blood. It plays a vital role in supplying oxygen and nutrients to the body’s tissues and removing waste products. Proper blood flow is crucial for tissue health and healing.
Venous Insufficiency: A Leading Cause of Leg Ulcers
One of the primary causes of leg ulcers is venous insufficiency. This condition occurs when the valves in the veins of the legs become damaged or weakened, leading to poor blood circulation and the accumulation of blood in the lower extremities. Over time, this increased One of the primary causes of leg ulcers is venous insufficiency.
This condition occurs when the valves in the veins of the legs become damaged or weakened, leading to poor blood circulation and the accumulation of blood in the lower extremities. Over time, this increased pressure in the veins can result in the development of ulcers.
Risk Factors for Venous Insufficiency
Several factors contribute to the development of venous insufficiency and, consequently, leg ulcers.
These risk factors include:
- Age: As we age, the veins lose their elasticity, making them more prone to valve damage and blood pooling.
- Obesity: Excessive weight puts increased pressure on the veins, impairing their ability to function properly.
- Pregnancy: Hormonal changes and the pressure of the growing uterus on the veins can lead to venous insufficiency.
- Family History: A genetic predisposition to weak vein valves can increase the likelihood of developing venous insufficiency.
- Sedentary Lifestyle: Lack of physical activity can hinder blood circulation and contribute to venous insufficiency.
- Previous Blood Clots: A history of deep vein thrombosis (DVT) or other blood clotting disorders can damage the veins, leading to insufficiency.
Symptoms of Venous Insufficiency
Recognizing the signs of venous insufficiency is crucial for early intervention.
Common symptoms include:
- Swelling in the lower legs, ankles, and feet
- Aching or throbbing pain in the legs, especially after prolonged standing or sitting
- Varicose veins, which are swollen and twisted veins visible beneath the skin
- Itching or a feeling of heaviness in the legs
- Skin discoloration, such as redness or brownish pigmentation
- Slow-healing wounds or ulcers on the lower leg, particularly around the ankle area
Arterial Insufficiency: Another Significant Cause of Leg Ulcers
While venous insufficiency is a common cause of leg ulcers, arterial insufficiency can also contribute to their development. Arterial insufficiency occurs when there is inadequate blood flow through the arteries, depriving the tissues of necessary oxygen and nutrients. Without a proper blood supply, the skin and underlying tissues become vulnerable to injury and slow wound healing.
Risk Factors for Arterial Insufficiency
Several factors increase the risk of arterial insufficiency and subsequent leg ulcers:
- Smoking: Smoking damages the arteries, leading to narrowed blood vessels and reduced blood flow.
- Diabetes: Uncontrolled diabetes can damage blood vessels, increasing the risk of arterial insufficiency.
- High Blood Pressure: Hypertension can cause arterial damage and impair blood flow.
- High Cholesterol: Elevated cholesterol levels can contribute to the formation of plaque in the arteries, restricting blood flow.
- Peripheral Artery Disease: Atherosclerosis, a condition characterized by the buildup of fatty deposits in the arteries, can lead to arterial insufficiency.
Symptoms of Arterial Insufficiency
Arterial insufficiency often manifests with distinct symptoms, including:
- Leg pain, especially during physical activity and relieved by rest
- Cold feet or legs
- Pale or bluish skin discoloration
- Weak or absent pulses in the feet and legs
- Slow-healing or non-healing wounds or ulcers on the lower leg or foot
- Hair loss or thinning on the legs and feet
Diabetes and Leg Ulcers
Diabetes is a chronic condition that can significantly contribute to the development of leg ulcers. Individuals with diabetes are at a higher risk of developing ulcer
How Diabetes Contributes to Leg Ulcers
In diabetes, high blood sugar levels can lead to damage to the blood vessels, particularly the smaller ones supplying the legs and feet. This vascular damage, combined with neuropathy, reduces blood flow and impairs sensation in the extremities.
As a result, minor injuries such as cuts, blisters, or sores may go unnoticed and fail to heal properly. Over time, these non-healing wounds can progress into ulcers.
Additionally, diabetes weakens the immune system, making it more difficult for the body to fight off infections. When an ulcer forms, it becomes susceptible to bacterial growth and increases the risk of complications such as cellulitis or even deep tissue infections.
Preventing and Managing Diabetic Leg Ulcers
Prevention and proper management are crucial in reducing the incidence of leg ulcers in individuals with diabetes.
Some key strategies include:
- Maintaining good blood sugar control: Keeping blood glucose levels within the target range helps promote better wound healing and reduces the risk of complications.
- Regular foot care: Inspecting the feet daily, washing them with lukewarm water, and keeping the skin moisturized can help prevent skin breakdown and identify any abnormalities or wounds at an early stage.
- Wearing appropriate footwear: Choosing comfortable shoes that fit well and provide adequate support can help prevent pressure points and reduce the risk of developing ulcers.
- Regular check-ups: Routine visits to healthcare professionals allow for early detection of any foot or leg issues, allowing for prompt intervention and prevention of ulcers.
Infections and Wound Healing
Infections play a significant role in the progression and delayed healing of leg ulcers. When an ulcer occurs, it creates an entry point for bacteria, leading to infection. Furthermore, the presence of infection can impair the natural wound-healing process.
Infection as a Cause of Leg Ulcers
Leg ulcers can become infected through various means, including exposure to bacteria in the environment or from the individual’s own skin flora. Poor wound care, inadequate hygiene, and underlying conditions such as diabetes or compromised immune function can increase the likelihood of infection.
The Importance of Proper Wound Care
Proper wound care is essential for preventing and managing leg ulcers.
The following measures are crucial:
- Cleaning the wound: Gently washing the ulcer with mild soap and water or a saline solution helps remove debris and reduce the risk of infection.
- Applying appropriate dressings: Dressings protect the wound, facilitate a moist environment conducive to healing, and may contain antimicrobial properties to prevent or treat the infection.
- Managing exudate: Leg ulcers may produce varying amounts of fluid, and appropriate dressings should be chosen to absorb excess exudate while maintaining a moist wound environment.
- Debridement: In some cases, debridement may be necessary to remove dead or non-viable tissue from the wound bed, promoting the growth of healthy tissue.
- Antibiotics: If an infection is present, healthcare professionals may prescribe antibiotics to target the specific bacteria causing the infection.
Other Contributing Factors
In addition to venous insufficiency, arterial insufficiency, and diabetes, several other factors can contribute to the development of leg ulcers. These include obesity, peripheral vascular disease (PVD), and smoking.
Obesity and its Impact on Leg Ulcers
Peripheral Vascular Disease and Leg Ulcers
Peripheral vascular disease (PVD) refers to the narrowing or blockage of blood vessels outside of the heart and brain. This condition can significantly impact blood flow to the legs, increasing the risk of ulcers.
PVD is often caused by atherosclerosis, where plaque buildup narrows the arteries and restricts blood flow. Reduced blood supply to the legs can result in tissue damage and non-healing wounds, which may progress to leg ulcers.
Smoking and Leg Ulcers
Smoking is a detrimental habit that can have severe implications for vascular health. The chemicals in tobacco smoke damage blood vessels, making them more susceptible to narrowing, blood clot formation, and decreased blood flow.
Smoking also impairs wound healing and weakens the immune system, making smokers more prone to infections. Consequently, smoking significantly increases the risk of developing leg ulcers and hampers the healing process.
Diagnosing Leg Ulcers
Diagnosing the underlying cause of leg ulcers is crucial for effective treatment and management. Healthcare professionals employ various methods to assess and diagnose leg ulcers:
Clinical Evaluation
During a clinical evaluation, a healthcare provider will examine the ulcer and assess its characteristics, such as size, location, and appearance. They will also consider the patient’s medical history, risk factors, and symptoms to determine the likely cause of the ulcer.
Imaging and Laboratory Tests
In some cases, additional tests may be necessary to support the diagnosis. Doppler ultrasound, for instance, can assess blood flow in the legs and identify any vascular abnormalities. Laboratory tests, including blood tests, can help detect underlying conditions such as diabetes or infection.
Treating Leg Ulcers
The treatment of leg ulcers focuses on addressing the underlying cause, promoting wound healing, and preventing complications. The following approaches are commonly employed:
Compression Therapy
Compression therapy is a cornerstone in managing venous leg ulcers. It involves applying specially designed stockings or bandages to exert external pressure on the veins, promoting blood flow and reducing swelling. Compression therapy helps improve circulation, aids in wound healing, and prevents ulcer recurrence.
Wound Care and Dressings
Proper wound care is essential for promoting healing and preventing infection. Healthcare professionals may recommend various types of dressings, such as hydrogels, foam dressings, or alginate dressings, depending on the characteristics of the ulcer. Regular cleaning, debridement of dead tissue, and appropriate dressings are crucial for maintaining a clean and optimal wound-healing environment.
Surgical Interventions
In certain cases, surgical interventions may be necessary to address underlying vascular issues or remove non-healing tissue. Procedures such as vein ligation, vein stripping, or angioplasty may be performed to improve blood flow and facilitate wound healing.
Adjunctive Therapies
Additional therapies may be used in conjunction with conventional treatments to enhance healing and manage leg ulcers. These may include growth factors, skin substitutes, negative pressure wound therapy, or hyperbaric oxygen therapy, depending on the individual case and the recommendation of the healthcare provider
Preventing Leg Ulcers
Prevention is key when it comes to leg ulcers, especially for individuals at risk. Here are some important preventive measures to consider:
Maintaining a Healthy Lifestyle
- Engage in regular exercise: Physical activity promotes good circulation and helps maintain a healthy weight, reducing the risk of leg ulcers.
- Follow a balanced diet: A nutritious diet rich in fruits, vegetables, whole grains, and lean proteins supports overall vascular health and can lower the risk of developing ulcers.
- Manage chronic conditions: Properly managing conditions such as diabetes, hypertension, and high cholesterol can help minimize their impact on vascular health.
Foot and Leg Care
- Inspect feet daily: Regularly examine the feet for any cuts, sores, or abnormalities. Seek prompt medical attention for any concerning findings.
- Practice proper hygiene: Keep the feet clean and dry to prevent infections. Use mild soap and warm water, and thoroughly dry the feet, especially between the toes.
- Moisturize the skin: Regularly apply moisturizer to prevent dryness and cracking, which can increase the risk of ulcers.
- Trim toenails carefully: Cut toenails straight across and avoid cutting them too short to prevent ingrown toenails and potential skin injuries.
- Wear comfortable shoes: Opt for well-fitting shoes made of breathable materials to avoid pressure points and promote good circulation. Avoid high heels and tight-fitting footwear.
There are many causes of leg ulcers, but they all have the same basic underlying cause: the underlying condition that causes vascular problems.
Fortunately, arterial ulcers are rare and much easier to treat than other types of ulcers. Vascular (arterial) surgeons can help with this condition. Other causes of leg ulcers include chronic venous insufficiency and varicose veins.
Varicose veins
There are several treatments to help reduce leg ulcers caused by varicose veins. Elevating the legs can help, as can taking medication such as anti-coagulants and diuretics. Other treatments include anti-inflammatory medications that thin blood. Laser surgery is another treatment that uses strong surges of light to close the vein.
However, these treatments do not address the underlying cause of varicose veins. Treatment for leg ulcers typically targets the vein responsible for the ulcer. Physicians will determine which treatment is best for each individual patient.
This may involve ablation,microphlebectomy, or sclerotherapy. The goal is to redirect the blood flow from the ulcer-causing vein to a healthier one. Increased blood flow to the leg will result in improved oxygen and nutrients to the ulcerative area, and eventually, lead to healing.
Chronic venous insufficiency
The best treatment for chronic venous insufficiency is elevating the leg above heart level. This helps reduce swelling and improves blood flow in the leg veins, speeding up the healing process.
It is the most effective treatment, but a footstool does little to improve the drainage of blood from the leg. Leg elevation may be the only treatment needed in mild cases of chronic venous insufficiency.
More severe cases may require surgical management. Treatment for chronic venous insufficiency depends on the symptoms and severity of the disease. Compression stockings and elevating the leg may help. Some people may also benefit from good skin care and exercise.
However, treatment for chronic venous insufficiency is not without risks. The condition may reoccur in the future. But there are ways to improve symptoms and improve the quality of life for those with venous insufficiency.
Arterial ulcers
The main cause of a leg or foot ulcer is blocked blood flow. This causes blood to pool in the affected area and leaks blood cells and fluid. The tissue dies and an ulcer forms. This condition may require amputation in severe cases.
Proper care and antibiotics can help to heal an ulcer, but treating the underlying cause is always recommended. Here are the symptoms and causes of arterial leg ulcers. The main treatment for an arterial leg ulcer involves increasing the blood supply to the affected area.
Compression therapy, which involves applying a bandage to the affected area, helps improve blood flow. Painkillers are also prescribed. Elevating the affected leg will help to reduce the discomfort caused by an ulcer.
Surgery may also be necessary if the ulcer becomes too septic or infected. Treatment for leg ulcers can range from medication to surgery, depending on the severity of the condition.
Compression bandages
Leg ulcers are often caused by underlying conditions. While there is no cure for leg ulcers, there are several ways to treat them, including using compression bandages.
Compression bandages are made of elastic stretch fabric and improve blood circulation in the leg, preventing blood clots and reducing fluid build-up. Keeping the affected leg elevated while at rest is a good idea as well. If the ulceration is arterial, then it should be evaluated by a vascular surgeon and treated accordingly.
Then, if necessary, surgery can be performed. In contrast, venous ulcers can be managed with conservative measures, though in some cases, surgery may be necessary to correct an underlying physiological disorder. Despite these risks, the main goal of treatment is to promote improved blood flow to the affected area and promote healing.
Shave therapy
The most common treatment for leg ulcers is shaving therapy. While the shave therapy procedure involves skin grafting, tangential excision is a better choice for trophically destroyed tissues.
This procedure is also effective in accelerating the healing process. The surgeon may remove the crural fascia, which is optional and controversial. The surgical technique may also include a skin graft from the underlying dermis, which is called autologous. Patients undergoing shave therapy have seen promising results.
The initial pain was less than four points on a 0-10 scale, and it was hardly noticeable during the first dressing change. It has been proven that shave therapy is a safe, effective treatment for leg ulcers.
However, there are some risks. In addition to a possible risk of allergic contact eczema, patients are at increased risk of developing type IV allergies.
Additionally, many ask
What is the most expedient method for healing an ulcer on the leg?
It’s possible that the following suggestions will speed up the healing process for your ulcer.
Make an effort to stay active by going for walks on a regular basis.
Keep the leg that is hurting you up at all times, including when you are sitting or lying down. Perform regular leg exercises by moving your feet up and down and turning them at the ankles. This will help strengthen your legs.
What is the primary contributor to the development of chronic leg ulcers?
The illness of the veins in the leg is the underlying condition that is responsible for chronic leg ulcers more often than any other. Over two-thirds of all leg, ulcers are caused by venous illness, making it the most common cause. It is possible that in some instances two or more conditions are simultaneously causing damage to the body.
What does it mean if you have ulcers in your legs?
Ulcers of the leg are incapacitating and significantly lower the quality of life for patients. Venous disease, arterial disease, and neuropathy are the most frequent underlying conditions. Infectious infections, metabolic problems, and hematological disorders are some of the less common causes of this condition.
What are the early warning indicators if someone has a leg ulcer?
Pain, itching, and swelling in the leg that is afflicted are some of the signs that someone has a venous leg ulcer. In addition to this, the skin around the ulcer may become discolored or thickened, and the wound itself may create a discharge with a putrid odor.
If you suspect that you have a leg ulcer, you should make an appointment with your primary care physician as soon as possible so that the ulcer can be treated by a specialist.
Are leg ulcers serious?
An ulcer on your leg that takes a very long time to cure is known as a venous skin ulcer. This is typically caused by poor blood circulation in the limb. They may just last a few weeks or they may persist for many years.
They are sometimes referred to as “venous leg ulcers” by medical professionals. If you choose not to get treatment for them, they may eventually develop into more serious issues.
Can you tell me about the most recent treatment for leg ulcers?
The use of topical oxygen therapy, also known as TOT, is a relatively new technique for the treatment of venous leg ulcers that are difficult to heal. It is not necessary to have a full-body compression chamber in order to use TOT because it is delivered directly to the wound.
Ulcers on the leg provide a risk for cancer.
Squamous cell carcinoma is the most prevalent kind of cancer that can develop from chronic leg ulcers, which can develop into any of the other types of chronic leg ulcers.
If not diagnosed at an early stage, these ulcers, which are also known as Marjolin’s ulcers, have a terrible prognosis and a high potential for spreading to other parts of the body.
How can you protect yourself from getting leg ulcers?
Dropping some pounds People who are overweight are at a much-increased risk of developing venous ulcers. It is recommended that you participate in regular physical activity and consume a diet that is both nutritious and balanced if you want to shed some pounds.
In addition to this, you should try to avoid sitting or standing for extended periods of time. Keeping your legs elevated for as much of the time as you can also be beneficial.
What are the consequences of leg ulcers that refuse to heal?
The increased likelihood of infection that comes with having an exposed sore is what sets venous leg ulcers different from other types of illnesses.
She recommends making an appointment with a physician or nurse practitioner as soon as possible if you have a wound that hasn’t healed after two to three weeks. They will do an assessment and then make a referral for you to a wound care center.
Ulcers of the leg might result in amputation.
Leg ulcers are dangerous. In point of fact, they are even capable of causing amputations. The good news is that although leg ulcers can result in the loss of a portion of the leg due to amputation, these persistent sores almost seldom result in the loss of a foot or a leg. 15 Aug 2018
Conclusion
In conclusion, leg ulcers are primarily caused by poor circulation in the legs, often resulting from chronic venous insufficiency. This condition leads to blood pooling and increased pressure, damaging the skin and tissues and ultimately causing ulcers.
Other factors such as arterial disease, diabetes, and inflammatory conditions can also contribute to the development of leg ulcers. Secondary factors like infections, trauma, obesity, smoking, and immobility can further exacerbate the condition.
Addressing the underlying cause and managing these factors are vital for the effective treatment and prevention of leg ulcers. It is important to seek medical attention and follow a comprehensive care plan to promote healing and improve the quality of life for individuals with leg ulcers.
Health
Hair Gummies: A Trend Worth Your Time or Just Another Health Fad?

Hair Gummies: A Trend Worth Your Time or Just Another Health Fad?
In recent years, hair gummies have taken the health and beauty world by storm, boasting promises of luscious locks and a speedy route to hair health.
But with an array of products flooding the market, it’s essential to separate fact from fiction.
Are these colorful, chewy supplements a miracle solution for your hair troubles, or are they simply a trendy snack with little efficacy?
In this comprehensive article, we will explore the science behind hair gummies, their ingredients, potential benefits, and the questions surrounding their effectiveness.
Understanding Hair Health
The Basics of Hair Growth
To fully grasp the impact of hair gummies, it’s vital to understand how hair grows.
Each strand of hair goes through three main phases:
- Anagen Phase: This is the active growth phase, which can last several years. The length of this phase varies among individuals.
- Catagen Phase: A transitional phase lasting a few weeks, where hair growth slows, and the hair follicle shrinks.
- Telogen Phase: The resting phase, lasting a few months before the hair falls out, making way for new growth.
Hair health is influenced by a variety of factors, including genetics, hormones, diet, and overall health.
As such, a balanced approach to hair care, encompassing nutrition, proper hair care routines, and avoiding damaging practices, is essential.
Common Causes of Hair Issues
Hair loss or poor hair health can arise from numerous factors:
- Nutritional Deficiencies: A lack of essential vitamins and minerals can hinder hair growth.
- Hormonal Changes: Conditions like pregnancy, menopause, and thyroid disorders can significantly affect hair health.
- Stress: Chronic stress can trigger hair loss through a condition known as telogen effluvium.
- Medical Conditions: Certain diseases and medications can also contribute to hair loss.
What Are Hair Gummies?
Hair gummies are dietary supplements designed to promote hair health.
They are usually made with a combination of vitamins, minerals, and sometimes botanical extracts, often marketed as a convenient and tasty alternative to traditional vitamin pills.
Key Ingredients in Hair Gummies
While formulations vary, here are some common ingredients found in hair gummies:
- Biotin: A B-vitamin known for its role in hair and nail health. Biotin deficiencies can lead to brittle hair and hair loss.
- Vitamins A, C, and E: Antioxidants that help protect hair from oxidative stress, promoting a healthy scalp and hair growth.
- Folic Acid: Important for cell growth and regeneration, folic acid is believed to support healthy hair follicles.
- Zinc: Plays a role in hair tissue growth and repair, making it a crucial mineral for maintaining healthy hair.
- Collagen: An essential protein for skin elasticity that may also benefit hair strength and growth.
Do Hair Gummies Really Work?
The Science Behind Hair Gummies
While the ingredients in hair gummies are known to contribute to hair health, the question remains:
Do they work as effectively as claimed?
Here’s what the research suggests:
- Biotin: Studies have shown that biotin can improve hair thickness in those with deficiencies, but most people get sufficient biotin from their diet. Supplementing with biotin may not yield significant benefits for individuals who are not deficient.
- Vitamins and Minerals: Research indicates that vitamins A, C, D, E, and minerals like zinc and iron play a role in maintaining healthy hair. However, simply taking these vitamins in gummy form doesn’t guarantee results unless there’s a deficiency present.
- Collagen: Some studies suggest that collagen supplements can improve hair and skin health by providing amino acids essential for protein synthesis. However, more research is needed to establish direct benefits for hair growth.
User Experiences and Anecdotes
While anecdotal evidence often highlights positive experiences with hair gummies, it’s important to approach these testimonials with caution. Individual results may vary, and factors such as diet, overall health, and genetics play significant roles in hair health.
Potential Benefits of Hair Gummies
While not a miracle solution, hair gummies may offer certain benefits:
- Convenient Form: For those who struggle with swallowing pills, gummies provide a palatable alternative.
- Added Nutrients: If you have a deficiency in specific vitamins or minerals, hair gummies can supplement your diet effectively.
- Increased Awareness of Nutrition: Taking supplements can prompt individuals to pay more attention to their overall nutritional intake.
- Improved Hair Appearance: Users may notice shinier and healthier-looking hair due to the vitamins and antioxidants present in these products.
Are There Risks?
While hair gummies are generally safe, there are some considerations to keep in mind:
- Overconsumption: Gummies are often flavored and sweetened, which may lead to overconsumption and potential digestive issues.
- Sugar Content: Many gummies contain added sugars, which can contribute to other health problems if consumed excessively.
- Interactions with Other Supplements: If you’re taking other vitamins or supplements, it’s essential to ensure you’re not exceeding recommended doses, particularly for fat-soluble vitamins like A and E, which can accumulate in the body.
What Experts Say
Dermatologists and nutritionists often emphasize a balanced diet over reliance on supplements.
They suggest that whole foods—rich in vitamins, minerals, and healthy fats—are the best source for hair health.
Foods such as leafy greens, nuts, seeds, fish, and eggs can provide essential nutrients without the added sugars and potential downsides of gummies.
Conclusion:
Fad or Fact?
In conclusion, hair gummies may not be the ultimate solution for hair health, but they can serve as a helpful supplement for those with specific nutritional deficiencies.
They are convenient and may improve the overall appearance of hair for some users. However, it’s crucial to approach them with realistic expectations and prioritize a balanced diet rich in whole foods.
If you’re considering adding hair gummies to your routine, consult with a healthcare provider or nutritionist to ensure you’re making an informed decision that aligns with your health goals.
FAQs
1. Can hair gummies replace a balanced diet?
No, hair gummies are supplements and should not replace a balanced diet. They can help fill nutritional gaps but should be taken alongside a healthy eating plan.
2. How long does it take to see results from hair gummies?
Results vary, but users may start noticing improvements in hair texture and appearance after 4-12 weeks of consistent use.
3. Are hair gummies safe for everyone?
Most hair gummies are safe for general use; however, individuals with specific health conditions or allergies should consult a healthcare professional before taking them.
4. Can I take hair gummies with other supplements?
Yes, but be cautious of total vitamin and mineral intake to avoid exceeding recommended daily allowances. Consult with a healthcare provider for personalized advice.
5. Are there any side effects of hair gummies?
Some users may experience digestive issues, allergic reactions, or headaches due to high sugar content or specific ingredients. It’s best to start with a small dose to assess tolerance.
References:
Health
Understanding the Spine: Common Conditions and Effective Solutions
Understanding the Spine: Common Conditions and Effective Solutions
The spine is an essential structure in the human body, acting as a central pillar that supports our posture, facilitates movement, and protects the spinal cord.
Despite its importance, many individuals experience various spine-related conditions that can impact their quality of life.
In this comprehensive article, we will explore common spinal conditions, their causes, symptoms, and effective methods to address them.
What is the Spine?
The spine, also known as the vertebral column, is composed of 33 vertebrae arranged in a flexible yet sturdy structure.
It serves several critical functions:
- Support: The spine supports the head and allows for an upright posture.
- Protection: It encases and protects the spinal cord, a crucial component of the central nervous system.
- Mobility: The spine allows for a wide range of movements, including bending, twisting, and turning.
- Weight Distribution: It helps distribute weight and absorbs shock during activities like walking or running.
Understanding the structure and function of the spine is vital for recognizing and addressing the conditions that can affect it.
Common Spinal Conditions
Several conditions can adversely impact the spine, leading to pain, discomfort, and reduced mobility. Here are some of the most common spinal conditions:
1. Herniated Discs
A herniated disc occurs when the soft inner material of a spinal disc bulges out through a tear in the outer layer. This can compress nearby nerves, leading to pain, numbness, or weakness in the arms or legs.
Causes:
- Age-related degeneration
- Heavy lifting or sudden movements
- Trauma or injury
Symptoms:
- Localized back pain
- Radiating pain to the limbs
- Numbness or tingling
Treatment:
- Physical therapy
- Pain management through medications
- In severe cases, surgery may be required.
2. Spinal Stenosis
Spinal stenosis is the narrowing of the spinal canal, which can lead to pressure on the spinal cord and nerves. This condition often occurs in the cervical (neck) or lumbar (lower back) regions.
Causes:
- Age-related changes in the spine
- Osteoarthritis
- Herniated discs
Symptoms:
- Pain or cramping in the legs
- Weakness or numbness
- Difficulty walking or standing for extended periods
Treatment:
- Physical therapy and exercise
- Medications for pain relief
- In some cases, surgical decompression may be necessary.
3. Scoliosis
Scoliosis is an abnormal curvature of the spine, often appearing in childhood or adolescence. While many cases are mild, severe scoliosis can lead to complications.
Causes:
- Idiopathic (unknown cause)
- Congenital (present at birth)
- Neuromuscular conditions
Symptoms:
- Uneven shoulders or hips
- Visible curvature of the spine
- Back pain
Treatment:
- Monitoring and observation for mild cases
- Bracing for growing children
- Surgery for severe curvatures.
4. Osteoporosis
Osteoporosis is a condition characterized by weakened bones, making them more susceptible to fractures. This is particularly concerning for the vertebrae, which can lead to compression fractures.
Causes:
- Aging
- Hormonal changes
- Lack of calcium and vitamin D
Symptoms:
- Height loss
- Back pain due to fractures
- A stooped posture
Treatment:
- Medications to strengthen bones
- Nutritional supplements (calcium and vitamin D)
- Weight-bearing exercises to improve bone density.
5. Degenerative Disc Disease
Degenerative disc disease refers to the wear and tear of spinal discs over time, leading to pain and reduced flexibility.
Causes:
- Age-related degeneration
- Repetitive stress on the spine
- Genetics
Symptoms:
- Chronic back pain
- Pain that worsens with movement
- Possible radiating pain in the limbs
Treatment:
- Physical therapy and exercise
- Pain management strategies
- Surgical options for severe cases.
Preventing Spinal Conditions
While some spinal conditions are unavoidable due to genetics or aging, many can be prevented or mitigated through healthy lifestyle choices.
Here are some preventative measures:
1. Maintain Good Posture
Proper posture helps reduce strain on the spine. When sitting, keep your back straight, shoulders relaxed, and feet flat on the ground. When standing, distribute your weight evenly on both feet.
2. Stay Active
Regular physical activity strengthens the muscles that support the spine and improves flexibility. Aim for a balanced routine that includes strength training, aerobic exercise, and stretching.
3. Ergonomic Work Environment
If you spend long hours at a desk, ensure your workspace is ergonomically designed. Adjust your chair, desk height, and computer monitor to reduce strain on your back and neck.
4. Healthy Weight Management
Maintaining a healthy weight reduces stress on the spine and helps prevent conditions like degenerative disc disease and spinal stenosis.
5. Avoid Smoking
Smoking impairs blood flow and can lead to spinal degeneration. Quitting smoking can improve overall health and reduce the risk of spinal issues.
Effective Treatments for Spinal Conditions
If you experience spine-related pain or discomfort, it’s essential to consult a healthcare professional for a proper diagnosis and treatment plan.
Here are some common treatment options:
1. Physical Therapy
Physical therapists develop personalized exercise programs to strengthen the back muscles, improve flexibility, and alleviate pain. They may also use techniques like ultrasound or electrical stimulation to manage discomfort.
2. Medications
Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can help manage mild to moderate pain. Prescription medications may be necessary for more severe pain or inflammation.
3. Injections
Corticosteroid injections can reduce inflammation and provide temporary relief for conditions like herniated discs or spinal stenosis. These are typically used when other treatments have failed.
4. Surgery
In severe cases, surgery may be necessary to relieve pressure on the spinal cord or nerves. Common surgical procedures include discectomy (removal of herniated disc material), spinal fusion, and laminectomy (removal of part of the vertebra).
5. Alternative Therapies
Complementary treatments like acupuncture, chiropractic care, and massage therapy may provide relief for some individuals. Always consult with a healthcare professional before trying alternative therapies.
Conclusion
Understanding the spine and its common conditions is crucial for maintaining a healthy lifestyle and preventing potential issues.
By recognizing symptoms early and seeking appropriate treatment, individuals can address spinal conditions effectively.
Implementing preventative measures, such as maintaining good posture and staying active, can significantly reduce the risk of developing spine-related issues.
Prioritize your spinal health, consult with professionals when necessary, and take proactive steps to ensure a healthy and pain-free back.
FAQs
1. What are the common symptoms of spinal conditions?
Common symptoms include localized back pain, radiating pain in the limbs, numbness, tingling sensations, and difficulty with movement.
2. How can I improve my posture while working?
To improve your posture at work, adjust your chair and desk height, use a supportive chair, and ensure your computer screen is at eye level.
3. Can physical therapy help with spinal conditions?
Yes, physical therapy can help strengthen back muscles, improve flexibility, and alleviate pain associated with various spinal conditions.
4. When should I see a doctor for back pain?
If you experience persistent back pain that does not improve with rest, is accompanied by numbness or weakness, or interferes with daily activities, it’s essential to see a doctor.
5. Are there lifestyle changes I can make to prevent spinal issues?
Yes, maintaining a healthy weight, staying active, practicing good posture, and avoiding smoking can help prevent spinal conditions.
References:
Health
Understanding the Causes of Premature Menopause in Women
-

 Trending Stories1 year ago
Trending Stories1 year agoCDC: 1 in 4 Americans Still COVID-Free by End of 2022
-

 Health5 years ago
Health5 years agoMeghan Trainor Shares Motivational New Song ‘Blink’
-

 Health6 months ago
Health6 months agoHow Do Pawpaw Seeds Support Cardiovascular Health?
-

 Health2 years ago
Health2 years agoHow Long Does Monkey Pox Last Before It Surfaces in the Body?
-

 Health3 years ago
Health3 years agoWhat Causes Swollen Body? Understanding Edema and its Triggers
-

 Health3 years ago
Health3 years agoNutrition and the Importance of a Fitness Program – 3 Things to Know
-

 Health3 years ago
Health3 years ago5 Weird Reasons Why Pimples Disappear After Marriage
-

 Health2 years ago
Health2 years agoHealth Benefits Of Pawpaw Seed? 7 Things To Know