Health
Understanding the Rapid Spread of Monkeypox’s New Strain Clade 1b
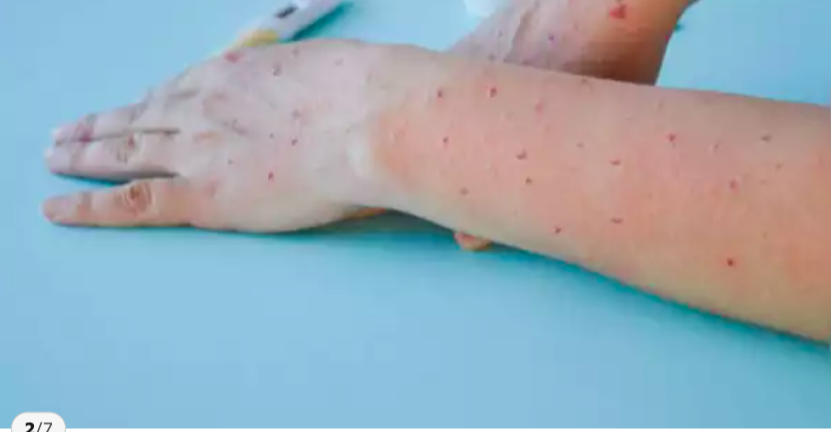
Understanding the Rapid Spread of Monkeypox’s New Strain Clade 1b: Key Facts on Transmission, Symptoms, Severity, and Vaccination
Monkeypox, a viral disease with symptoms resembling smallpox, has recently gained attention due to the emergence of a newstrain, Clade 1b.
This article delves into the essential details about this new variant, including how it spreads, its symptoms, its severity, and the current state of vaccinations.
Our goal is to provide a comprehensive and clear understanding of this evolving situation, enabling readers to stay informed and prepared.
Monkeypox, once a rare and somewhat obscure disease, has recently become a significant public health concern due to the emergence of new strains.
Among these, Clade 1b has been noted for its rapid spread and distinct characteristics.
As we navigate through the complexities of this variant, it is crucial to grasp the fundamentals of its transmission, symptoms, severity, and preventive measures, including vaccination.
Understanding Monkeypox Clade 1b
What is Monkeypox?
Monkeypox is a zoonotic virus belonging to the Orthopoxvirus genus, which also includes smallpox.
First identified in monkeys, it can infect humans through close contact with infected animals or individuals.
While it shares similarities with smallpox, monkeypox tends to be less severe and less transmissible.
Clade 1b Overview
Monkeypox has several clades (strains), with Clade 1b being the most recent and notable for its rapid spread.
This strain has shown increased transmissibility compared to previous clades, raising concerns among public health officials.
Transmission of Clade 1b
Modes of Transmission
Clade 1b spreads primarily through:
- Direct Contact: Contact with bodily fluids, skin lesions, or contaminated surfaces of an infected person.
- Respiratory Droplets: Prolonged face-to-face interaction can lead to transmission through respiratory droplets.
- Animal Contact: Infected animals, particularly rodents and primates, can transmit the virus to humans.
Environmental Factors
Transmission rates can also be influenced by environmental factors such as:
- Crowded Living Conditions: Higher transmission rates are observed in densely populated areas.
- Sanitation Practices: Poor hygiene and sanitation can facilitate the spread of the virus.
Symptoms of Monkeypox Clade 1b
Early Symptoms
The symptoms of Clade 1b may resemble those of other viral infections, making initial diagnosis challenging.
Early symptoms include:
- Fever: A sudden onset of high temperature.
- Headache: Severe headaches that can persist for days.
- Muscle Aches: Generalized muscle pain and discomfort.
- Fatigue: Extreme tiredness and weakness.
Rash and Skin Lesions
A defining feature of monkeypox is the rash, which typically progresses through several stages:
- Macules: Flat, discolored spots on the skin.
- Papules: Raised bumps.
- Vesicles: Fluid-filled blisters.
- Pustules: Pus-filled lesions that eventually crust over.
Severe Symptoms
In more severe cases, symptoms may include:
- Encephalitis: Inflammation of the brain, leading to neurological symptoms.
- Pneumonia: Infection of the lungs that can cause difficulty breathing.
- Secondary Infections: Bacterial infections that may complicate the healing process.
Severity of Clade 1b
General Outlook
Clade 1b has been associated with a higher transmission rate and more severe outcomes compared to other strains. However, the overall severity can vary widely among individuals.
Factors influencing severity include:
- Immune System Status: Individuals with weakened immune systems or pre-existing conditions may experience more severe symptoms.
- Age: Young children and elderly individuals are at higher risk of severe illness.
- Timeliness of Medical Care: Early medical intervention can significantly affect the outcome.
Mortality Rates
The mortality rate for Clade 1b is currently under study, but initial data suggest it may be higher than previous strains. Prompt medical attention and supportive care are crucial in reducing the risk of severe outcomes.
Vaccination and Prevention
Current Vaccines
Vaccination is a key strategy in controlling the spread of monkeypox.
The following vaccines are relevant:
- Smallpox Vaccine: The smallpox vaccine is effective against monkeypox due to the similarities between the viruses. It provides protection for those who have been recently vaccinated or who received it in the past.
- Monkeypox-Specific Vaccine: Research is ongoing into vaccines specifically targeting monkeypox, with several candidates showing promise in trials.
Vaccination Recommendations
Public health authorities recommend vaccination for:
- Healthcare Workers: Individuals who are at higher risk due to their profession.
- High-Risk Populations: People in areas experiencing outbreaks or those with frequent exposure to infected individuals.
Preventive Measures
In addition to vaccination, preventive measures include:
- Good Hygiene: Regular handwashing and use of hand sanitizers.
- Avoiding Contact: Minimizing close contact with individuals displaying symptoms or with infected animals.
- Isolation: Infected individuals should isolate themselves to prevent the spread of the virus.
Conclusion
The emergence of Monkeypox Clade 1b represents a significant challenge to global health. Its increased transmissibility and potential for severe outcomes highlight the importance of staying informed and proactive.
By understanding its transmission, symptoms, and preventive measures, individuals and communities can better protect themselves and mitigate the impact of this new strain.
FAQs
1. What makes Clade 1b different from other monkeypox strains?
Clade 1b is noted for its increased transmissibility and potentially more severe outcomes compared to other strains.
It spreads faster and may lead to more serious health issues, necessitating closer monitoring and enhanced preventive measures.
2. How can I tell if I have monkeypox or another viral infection?
Monkeypox often begins with flu-like symptoms and progresses to a distinct rash.
If you experience these symptoms, especially if you’ve been in contact with someone who has monkeypox or are in an outbreak area, seek medical advice for accurate diagnosis and testing.
3. Is the smallpox vaccine effective against Monkeypox Clade 1b?
Yes, the smallpox vaccine offers protection against monkeypox, including Clade 1b, due to the similarities between the two viruses.
However, its effectiveness may vary based on factors such as time since vaccination and individual health conditions.
4. Are there any new vaccines specifically for monkeypox?
Research is ongoing to develop and approve vaccines specifically targeting monkeypox.
Several candidates are in various stages of clinical trials, with some showing promising results in enhancing protection against monkeypox strains, including Clade 1b.
5. What should I do if I suspect I have monkeypox?
If you suspect you have monkeypox, contact a healthcare provider immediately. They can guide you through testing, diagnosis, and appropriate care.
In the meantime, practice good hygiene and avoid close contact with others to prevent spreading the virus.
References:
Health
The History and Impact of the Yellow Fever Epidemic

The History and Impact of the Yellow Fever Epidemic
Yellow fever is a viral hemorrhagic disease transmitted by infected mosquitoes, primarily the Aedes aegypti species. Known for its acute onset and severe symptoms, yellow fever has shaped the course of history through its devastating epidemics.
Understanding the origins, spread, and impact of yellow fever epidemics is crucial to appreciating the strides made in combating this deadly disease.
Origins of Yellow Fever
The origins of yellow fever trace back to Africa, where the virus likely evolved from primate hosts to humans. The disease was then transported to the Americas through the transatlantic slave trade in the 17th century.
The humid, tropical climate of the Caribbean and the southern United States provided an ideal environment for the Aedes aegypti mosquito to thrive, setting the stage for widespread outbreaks.
Major Yellow Fever Epidemics
Philadelphia Epidemic of 1793
One of the earliest and most severe yellow fever outbreaks occurred in Philadelphia in 1793. The epidemic struck during the summer, killing approximately 5,000 people—about 10% of the city’s population.
The outbreak led to mass panic and a significant exodus from the city. Medical professionals at the time, including Dr. Benjamin Rush, employed various treatments, though the true cause and transmission method of the disease were not yet understood.
New Orleans Epidemics of the 19th Century
New Orleans, with its warm climate and bustling port, experienced several devastating yellow fever epidemics throughout the 19th century.
The 1853 outbreak was particularly severe, resulting in over 9,000 deaths. The recurring nature of these epidemics significantly impacted the city’s development and economy.
Memphis Epidemic of 1878
The Memphis epidemic of 1878 was another catastrophic event. Originating from infected passengers arriving by steamboat, the outbreak spread rapidly, leading to over 5,000 deaths and causing the city’s population to plummet as residents fled.
This epidemic underscored the importance of understanding and controlling the spread of yellow fever.
Discovery of the Transmission Method
The late 19th century marked a turning point in the fight against yellow fever. Dr. Carlos Finlay, a Cuban physician, hypothesized that mosquitoes transmitted the disease.
This theory was later confirmed by the Walter Reed Commission in 1900, leading to significant advancements in controlling the spread of yellow fever.
This discovery emphasized the importance of mosquito control and paved the way for the development of effective public health measures.
The Role of Quarantine and Public Health Measures
In response to yellow fever outbreaks, quarantine measures and public health initiatives were implemented to curb the spread. Cities established quarantine stations and enacted sanitary regulations to reduce mosquito breeding grounds.
The success of these measures varied, but they laid the groundwork for modern public health practices.
Impact of Vaccination
The development of a yellow fever vaccine in the 1930s by Dr. Max Theiler revolutionized the fight against the disease. Theiler’s work earned him a Nobel Prize in 1951.
Vaccination campaigns have since been pivotal in preventing yellow fever outbreaks, particularly in endemic regions of Africa and South America.
Modern-Day Challenges and Efforts
Despite significant progress, yellow fever remains a threat in certain parts of the world. Urbanization, climate change, and population movement contribute to the risk of outbreaks. Modern efforts focus on vaccination, vector control, and surveillance to prevent and manage yellow fever.
Recent Outbreaks and Global Response
In recent years, yellow fever outbreaks have occurred in several African countries, including Angola and the Democratic Republic of Congo, highlighting the need for continued vigilance and international cooperation.
The World Health Organization (WHO) and other global health bodies have been instrumental in coordinating response efforts and ensuring vaccine availability.
Conclusion
The history of yellow fever epidemics underscores the importance of scientific discovery, public health initiatives, and international cooperation in combating infectious diseases.
From the devastating outbreaks of the past to modern efforts at prevention and control, the fight against yellow fever exemplifies the progress and challenges of global health.
FAQs About Yellow Fever
1. What are the symptoms of yellow fever?
Yellow fever symptoms typically include fever, chills, severe headache, back pain, general body aches, nausea, vomiting, fatigue, and weakness. In severe cases, it can cause jaundice, bleeding, and organ failure.
2. How is yellow fever transmitted?
Yellow fever is primarily transmitted through the bite of an infected Aedes aegypti mosquito. The mosquito becomes infected when it bites a person or monkey with the virus and can then transmit the virus to other humans through subsequent bites.
3. Is there a cure for yellow fever?
There is no specific cure for yellow fever. Treatment focuses on relieving symptoms and includes rest, fluids, and medications to reduce fever and pain. Severe cases may require hospitalization and supportive care.
4. Who should get vaccinated against yellow fever?
The yellow fever vaccine is recommended for people aged 9 months or older who are traveling to or living in areas at risk for yellow fever transmission. It is also recommended for laboratory personnel who might be exposed to the yellow fever virus.
5. How can yellow fever be prevented?
Yellow fever can be prevented through vaccination, using insect repellent, wearing protective clothing, and implementing mosquito control measures such as eliminating standing water where mosquitoes breed and using mosquito nets and screens.
References
Health
India’s Readiness for Mpox Prevention After Battling COVID-19: What Must Be Done?
Health
Why You Feel a Burning Sensation After Peeing: Common Causes and Solutions

Why You Feel a Burning Sensation After Peeing: Common Causes and Solutions
A burning sensation during or after urination is a discomforting issue that can affect anyone at any point in their life.
Whether you’re feeling mild irritation or intense pain, this condition often signals an underlying problem that requires attention. If you’ve ever wondered,
“Why does it burn when I pee?”
you’re not alone. In this article, we’ll explore the common causes behind this condition, how to address it, and ways to prevent it from occurring in the future.
What is a Burning Sensation After Urination?
A burning sensation after urination, also known as dysuria, is the feeling of pain, discomfort, or a stinging sensation during or right after you urinate.
While it can affect both men and women, it’s more commonly reported in women due to their shorter urethra.
Dysuria is a symptom, not a diagnosis, and it can indicate several underlying conditions.
Common Causes of Burning Sensation After Peeing
1. Urinary Tract Infection (UTI)
One of the most common reasons for a burning sensation after urination is a urinary tract infection (UTI).
UTIs occur when bacteria, most often Escherichia coli (E. coli), enter the urethra and multiply, leading to infection.
This infection can occur in any part of the urinary tract, including the bladder, kidneys, ureters, or urethra. Women are more prone to UTIs due to their shorter urethra.
Symptoms of UTIs:
- Frequent urge to urinate
- Pain or pressure in the lower abdomen
- Cloudy or strong-smelling urine
- Blood in the urine
2. Sexually Transmitted Infections (STIs)
Sexually transmitted infections, such as chlamydia, gonorrhea, and herpes, can cause a burning sensation during urination. These infections are usually contracted through sexual contact and may not always show symptoms right away, but when they do, dysuria is often one of the most common signs.
Symptoms of STIs:
- Unusual discharge
- Pain during intercourse
- Genital sores or rashes
3. Bladder Inflammation (Cystitis)
Cystitis refers to inflammation of the bladder, often caused by a bacterial infection but sometimes resulting from chemical irritants. In addition to causing a burning sensation, cystitis can lead to pelvic pain, frequent urination, and cloudy urine.
Causes of Cystitis:
- Bacterial infection
- Irritation from hygiene products (e.g., bubble baths, soaps)
- Radiation therapy or long-term catheter use
4. Kidney Stones
Kidney stones form when minerals in the urine crystallize and harden into stones, which can then pass into the ureters and bladder. When a stone is in the urethra, it can cause sharp, burning pain during urination.
Symptoms of Kidney Stones:
- Severe pain in the side and back
- Pain that radiates to the lower abdomen and groin
- Nausea and vomiting
- Blood in the urine
5. Dehydration
Not drinking enough water can lead to highly concentrated urine, which may irritate the urethra and cause a burning sensation. When you’re dehydrated, your urine is darker, more concentrated, and may contain more acidic waste products, which can cause discomfort.
Symptoms of Dehydration:
- Dark yellow urine
- Dry mouth and skin
- Dizziness or lightheadedness
6. Vaginal Infections
In women, vaginal infections such as yeast infections or bacterial vaginosis can result in a burning sensation when urinating. These infections often disturb the natural balance of bacteria in the vagina, causing inflammation and irritation.
Symptoms of Vaginal Infections:
- Thick, white, or watery discharge
- Itching and irritation in the vaginal area
- Redness and swelling
7. Prostatitis (In Men)
Prostatitis is the inflammation of the prostate gland in men, which can cause pain and burning sensations during urination. This condition can be either bacterial or non-bacterial.
Symptoms of Prostatitis:
- Difficulty urinating
- Pain in the lower abdomen, groin, or lower back
- Painful ejaculation
- Frequent urge to urinate
Other Causes to Consider
8. Chemical Irritation
Certain soaps, body washes, and feminine hygiene products can cause irritation to the urethral opening, leading to burning sensations. Be cautious when using heavily perfumed products around the genital area.
9. Diabetes
People with diabetes are more prone to urinary tract infections, which can lead to a burning sensation after urination. This is due to higher sugar levels in the urine, creating an environment where bacteria can thrive.
10. Medications
Certain medications, especially chemotherapy drugs, can irritate the bladder and urinary tract, causing discomfort during urination.
How to Diagnose the Cause of a Burning Sensation After Urinating
If you experience persistent burning after urinating, it’s important to see a healthcare provider for proper diagnosis. Your doctor may perform the following tests:
- Urine Test (Urinalysis): A urine sample can reveal signs of infection or other abnormalities.
- Blood Tests: These can help identify conditions like diabetes or kidney disease.
- Ultrasound or CT Scan: Imaging tests can detect kidney stones or structural abnormalities in the urinary tract.
- Swab Tests: For suspected STIs or vaginal infections, a swab of the genital area may be taken for testing.
Treatment Options for Burning Sensation After Urination
1. Antibiotics
If your burning sensation is due to a bacterial infection like a UTI or STI, antibiotics will be prescribed. It’s important to complete the full course of antibiotics, even if symptoms improve.
2. Hydration
Increasing water intake can help flush out bacteria and dilute your urine, reducing irritation. Aim to drink at least 8 glasses of water per day.
3. Pain Relievers
Over-the-counter pain relievers like ibuprofen or acetaminophen can help reduce inflammation and discomfort.
4. Topical Creams
For external irritation caused by soaps or other chemicals, using a mild, fragrance-free cream can help soothe the skin.
5. Cranberry Juice
Although research is mixed, some studies suggest that cranberry juice or supplements can help prevent UTIs by preventing bacteria from sticking to the walls of the urinary tract.
6. Sitz Baths
A sitz bath, which involves soaking the pelvic area in warm water, can provide relief from burning sensations and promote healing.
Prevention Tips
1. Practice Good Hygiene
Ensure you wipe from front to back after using the bathroom, especially for women, to prevent bacteria from spreading to the urethra. Regularly cleaning the genital area with mild, unscented soap can also help prevent irritation.
2. Urinate After Sexual Activity
Sexual intercourse can introduce bacteria into the urinary tract. Urinating after sex helps flush out any bacteria, reducing the risk of infection.
3. Stay Hydrated
Drinking plenty of water throughout the day can keep your urine dilute and help flush bacteria from your urinary tract.
4. Avoid Irritants
Avoid using heavily perfumed products like soaps, bubble baths, or feminine hygiene sprays in the genital area, as they can cause irritation.
5. Wear Breathable Fabrics
Opt for cotton underwear and loose-fitting clothing to keep the genital area dry and reduce the risk of infections.
When to See a Doctor
If your symptoms persist for more than a few days, worsen, or are accompanied by fever, back pain, or blood in your urine, you should seek medical attention. Ignoring a burning sensation after urination can lead to complications like kidney infections, which require more intensive treatment.
Conclusion
Experiencing a burning sensation after urination can be alarming, but understanding the causes and seeking timely treatment can help you find relief.
Whether it’s a urinary tract infection, sexually transmitted infection, or another underlying condition, identifying the root cause is essential.
By practicing good hygiene, staying hydrated, and avoiding irritants, you can reduce the chances of experiencing this uncomfortable symptom.
FAQs
1. Can dehydration cause a burning sensation after peeing?
Yes, dehydration can cause your urine to become more concentrated, which can irritate the urethra and lead to a burning sensation.
2. Is a burning sensation after urinating always a sign of infection?
No, while infections are a common cause, other factors such as irritation from soaps, dehydration, or even certain medications can lead to burning sensations without infection.
3. How long should a burning sensation after peeing last?
If the burning sensation is caused by a mild issue like dehydration or irritation, it should resolve within a day or two. However, if it persists longer or is accompanied by other symptoms, you should consult a doctor.
4. Can kidney stones cause burning sensations during urination?
Yes, kidney stones can cause pain and a burning sensation during urination, especially when the stone is passing through the urethra.
5. Should I avoid certain foods if I experience a burning sensation after peeing?
Yes, acidic foods like citrus fruits and caffeine can irritate the bladder and exacerbate burning sensations. Try to reduce your intake of such foods if you’re experiencing symptoms.
References:
(https://timesofindia.indiatimes.com/life-
-

 Trending Stories1 year ago
Trending Stories1 year agoCDC: 1 in 4 Americans Still COVID-Free by End of 2022
-

 Health5 years ago
Health5 years agoMeghan Trainor Shares Motivational New Song ‘Blink’
-

 Health2 years ago
Health2 years agoHow Long Does Monkey Pox Last Before It Surfaces in the Body?
-

 Health2 years ago
Health2 years agoWhat Causes Swollen Body? Understanding Edema and its Triggers
-

 Health5 months ago
Health5 months agoHow Do Pawpaw Seeds Support Cardiovascular Health?
-

 Health3 years ago
Health3 years agoNutrition and the Importance of a Fitness Program – 3 Things to Know
-

 Health3 years ago
Health3 years ago5 Weird Reasons Why Pimples Disappear After Marriage
-

 Health2 years ago
Health2 years agoHealth Benefits Of Pawpaw Seed? 7 Things To Know





