Health
Causes of Pain in Legs? 4 Things To Know

Last Updated on July 29, 2023 by Nurse Vicky
Causes of Pain in Legs: 4 Things To Know
Pain in the legs can be a distressing experience, affecting people of all ages and lifestyles. Whether it’s a dull ache, sharp pain, or throbbing sensation, leg pain can disrupt daily activities and reduce overall quality of life.
Understanding the causes of leg pain is crucial for proper diagnosis and treatment. In this comprehensive guide, we’ll delve into four important things you need to know about leg pain, its potential causes, and ways to alleviate discomfort.
Types of Leg Pain
Leg pain can manifest in various forms, each indicating different underlying issues. Common types of leg pain include:
Muscle Pain
Muscle pain, also known as myalgia, is a frequent cause of leg discomfort. It often results from overuse, muscle strain, or injury. Muscle pain can range from mild to severe and usually responds well to rest, stretching, and gradual re-introduction of physical activity.
Nerve Pain
Nerve pain, or neuropathy, occurs when nerves in the legs are damaged or compressed. Conditions such as sciatica or peripheral neuropathy can cause sharp shooting pain, tingling, or numbness in the legs. Treating nerve pain may involve addressing the underlying condition and using medications to manage symptoms.
Joint Pain
Joint pain in the legs is commonly associated with arthritis or other inflammatory conditions. The knees and hips are particularly susceptible to joint pain. Proper management of joint pain includes exercise, weight management, and anti-inflammatory medications.
Vascular Pain
Pain in the legs caused by vascular issues often includes conditions like deep vein thrombosis (DVT) or peripheral artery disease (PAD). These conditions can lead to swelling, cramping, and a feeling of heaviness in the legs. Treatment may involve blood-thinning medications, lifestyle changes, or surgical interventions.
Common Causes of Leg Pain
Understanding the underlying causes of leg pain is vital for effective treatment and prevention. Here are some common culprits:
Injury and Overuse
Sports injuries, accidents, or repetitive movements can strain muscles, ligaments, or tendons, leading to leg pain. Proper warm-up, stretching, and using protective gear can help prevent such injuries.
Arthritis
Arthritis is a degenerative joint condition that can cause inflammation and pain in the legs. Osteoarthritis and rheumatoid arthritis are the two most common types affecting the lower extremities.
Sciatica
Sciatica occurs when the sciatic nerve becomes compressed or irritated, leading to radiating pain from the lower back down to the legs. Poor posture and spinal issues often contribute to sciatica.
Blood Clots
Blood clots in the legs can obstruct blood flow, causing pain and swelling. Deep vein thrombosis (DVT) is a potentially serious condition that requires immediate medical attention.
Peripheral Neuropathy
Peripheral neuropathy is a result of nerve damage, often due to diabetes, alcoholism, or certain medications. It can lead to tingling, burning, or stabbing pain in the legs.
Varicose Veins
Varicose veins are enlarged, twisted veins that can cause pain and discomfort in the legs. They are more common in people who stand or sit for prolonged periods.
Peripheral Artery Disease
Peripheral artery disease (PAD) narrows arteries in the legs, reducing blood flow and causing leg pain, particularly during physical activity.
Diagnosis and Treatment
Proper diagnosis is essential to determine the cause of leg pain accurately. A healthcare professional will likely perform a physical examination and may recommend additional tests, such as X-rays, MRI, or blood work, to identify the underlying issue.
Conservative Approaches
Many cases of leg pain can be managed with conservative approaches, including:
- Rest and avoid strenuous activities to allow the body to heal.
- Ice and heat therapy to reduce inflammation and soothe sore muscles.
- Over-the-counter pain relievers to alleviate discomfort.
Physical Therapy
Physical therapy plays a crucial role in the rehabilitation of leg injuries. Therapists can design personalized exercise programs to strengthen muscles and improve flexibility.
Medications
In some cases, medications may be prescribed to manage pain, inflammation, or underlying conditions contributing to leg pain.
Invasive Treatments
For severe cases or when conservative methods prove ineffective, invasive treatments like injections or surgery may be considered.
Prevention Tips
Preventing leg pain involves adopting healthy habits and being mindful of potential risk factors.
Regular Exercise
Engaging in regular, low-impact exercises can strengthen leg muscles and improve overall circulation.
Proper Footwear
Wearing supportive and well-fitted shoes can reduce the strain on the feet and legs.
Weight Management
Maintaining a healthy weight can lessen the stress on the legs and joints.
Ergonomic Workspaces
If you have a sedentary job, ensure your workspace is ergonomically designed to minimize strain on the legs and back.
FAQs
Can leg pain be a sign of a more serious condition?
Yes, leg pain can be a symptom of underlying conditions like deep vein thrombosis (DVT), peripheral artery disease (PAD), or arthritis. Seeking medical attention is essential for proper evaluation.
What exercises can help alleviate leg pain?
Low-impact exercises like swimming, cycling, and yoga can help strengthen leg muscles and improve flexibility without putting excessive strain on joints.
Are there any natural remedies for leg pain?
Some natural remedies like applying ice packs, elevating the legs, and using essential oils for massage can provide temporary relief from leg pain.
Is it necessary to see a doctor for mild leg pain?
While mild leg pain may not always require immediate medical attention, it’s essential to monitor the pain and seek medical advice if it persists or worsens.
Can sitting for prolonged periods cause leg pain?
Yes, sitting for extended periods can lead to poor circulation and muscle fatigue, contributing to leg pain. Taking breaks and stretching can help alleviate this issue.
Can weight gain cause leg pain?
Yes, excess weight can put additional stress on the legs and joints, leading to pain and discomfort. Maintaining a healthy weight can alleviate this pressure.
Can leg pain be prevented in athletes and active individuals?
Yes, athletes and active individuals can reduce the risk of leg pain by warming up before exercise, using proper form, and allowing adequate time for rest and recovery.
For individuals with arthritis, lifestyle changes can significantly improve leg pain. Maintaining a healthy diet with anti-inflammatory foods, engaging in low-impact exercises, and using assistive devices, such as orthotic inserts or canes, can help manage arthritis-related leg pain.
Are there any specific home remedies for nerve-related leg pain?
While home remedies may not treat the underlying cause, they can provide relief from nerve-related leg pain. Some people find that applying warm compresses, practicing gentle stretches, or taking warm baths with Epsom salt can help alleviate discomfort.
Can leg pain during pregnancy be relieved naturally?
Yes, pregnancy-related leg pain can be managed naturally. Staying active, doing prenatal exercises, elevating the legs, and using pregnancy support pillows while sleeping can help reduce leg pain during pregnancy.
Conclusion
Leg pain is a common and often challenging issue that can affect anyone at any stage of life. Understanding the various types and causes of leg pain is essential for accurate diagnosis and appropriate treatment.
Whether it’s muscle pain from overuse, nerve pain due to compression, joint pain from arthritis, or vascular pain caused by blood flow issues, seeking professional medical advice is crucial.
In this long-form article, we’ve covered the key aspects of leg pain, providing valuable information to help readers understand, prevent, and manage leg pain effectively.
By following prevention tips, adopting a healthy lifestyle, and seeking medical guidance when necessary, individuals can work towards leading a life free from the burden of leg pain.
Remember, while this guide aims to provide valuable insights, it is not a substitute for professional medical advice. If you or someone you know is experiencing persistent or severe leg pain, it’s essential to consult a healthcare professional for personalized evaluation and treatment. Here’s to healthy, pain-free legs and a better quality of life for all!
References and Links
Health
6 Daily Habits to Naturally Lower Cholesterol Levels
Health
Understanding the Rapid Spread of Monkeypox’s New Strain Clade 1b
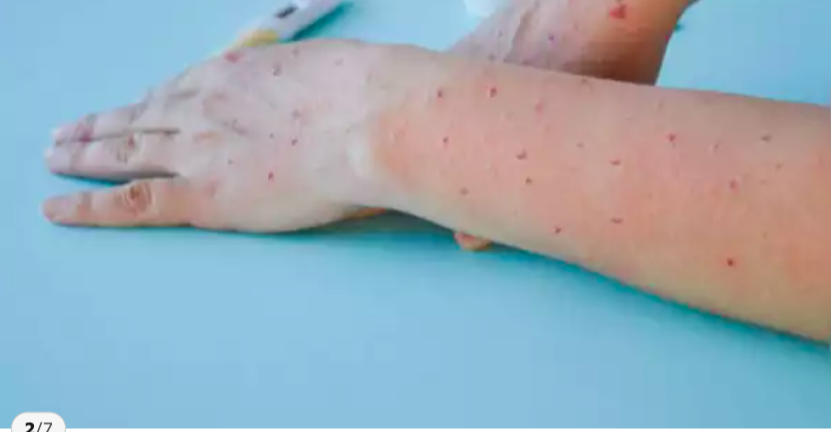
Understanding the Rapid Spread of Monkeypox’s New Strain Clade 1b: Key Facts on Transmission, Symptoms, Severity, and Vaccination
Monkeypox, a viral disease with symptoms resembling smallpox, has recently gained attention due to the emergence of a newstrain, Clade 1b.
This article delves into the essential details about this new variant, including how it spreads, its symptoms, its severity, and the current state of vaccinations.
Our goal is to provide a comprehensive and clear understanding of this evolving situation, enabling readers to stay informed and prepared.
Monkeypox, once a rare and somewhat obscure disease, has recently become a significant public health concern due to the emergence of new strains.
Among these, Clade 1b has been noted for its rapid spread and distinct characteristics.
As we navigate through the complexities of this variant, it is crucial to grasp the fundamentals of its transmission, symptoms, severity, and preventive measures, including vaccination.
Understanding Monkeypox Clade 1b
What is Monkeypox?
Monkeypox is a zoonotic virus belonging to the Orthopoxvirus genus, which also includes smallpox.
First identified in monkeys, it can infect humans through close contact with infected animals or individuals.
While it shares similarities with smallpox, monkeypox tends to be less severe and less transmissible.
Clade 1b Overview
Monkeypox has several clades (strains), with Clade 1b being the most recent and notable for its rapid spread.
This strain has shown increased transmissibility compared to previous clades, raising concerns among public health officials.
Transmission of Clade 1b
Modes of Transmission
Clade 1b spreads primarily through:
- Direct Contact: Contact with bodily fluids, skin lesions, or contaminated surfaces of an infected person.
- Respiratory Droplets: Prolonged face-to-face interaction can lead to transmission through respiratory droplets.
- Animal Contact: Infected animals, particularly rodents and primates, can transmit the virus to humans.
Environmental Factors
Transmission rates can also be influenced by environmental factors such as:
- Crowded Living Conditions: Higher transmission rates are observed in densely populated areas.
- Sanitation Practices: Poor hygiene and sanitation can facilitate the spread of the virus.
Symptoms of Monkeypox Clade 1b
Early Symptoms
The symptoms of Clade 1b may resemble those of other viral infections, making initial diagnosis challenging.
Early symptoms include:
- Fever: A sudden onset of high temperature.
- Headache: Severe headaches that can persist for days.
- Muscle Aches: Generalized muscle pain and discomfort.
- Fatigue: Extreme tiredness and weakness.
Rash and Skin Lesions
A defining feature of monkeypox is the rash, which typically progresses through several stages:
- Macules: Flat, discolored spots on the skin.
- Papules: Raised bumps.
- Vesicles: Fluid-filled blisters.
- Pustules: Pus-filled lesions that eventually crust over.
Severe Symptoms
In more severe cases, symptoms may include:
- Encephalitis: Inflammation of the brain, leading to neurological symptoms.
- Pneumonia: Infection of the lungs that can cause difficulty breathing.
- Secondary Infections: Bacterial infections that may complicate the healing process.
Severity of Clade 1b
General Outlook
Clade 1b has been associated with a higher transmission rate and more severe outcomes compared to other strains. However, the overall severity can vary widely among individuals.
Factors influencing severity include:
- Immune System Status: Individuals with weakened immune systems or pre-existing conditions may experience more severe symptoms.
- Age: Young children and elderly individuals are at higher risk of severe illness.
- Timeliness of Medical Care: Early medical intervention can significantly affect the outcome.
Mortality Rates
The mortality rate for Clade 1b is currently under study, but initial data suggest it may be higher than previous strains. Prompt medical attention and supportive care are crucial in reducing the risk of severe outcomes.
Vaccination and Prevention
Current Vaccines
Vaccination is a key strategy in controlling the spread of monkeypox.
The following vaccines are relevant:
- Smallpox Vaccine: The smallpox vaccine is effective against monkeypox due to the similarities between the viruses. It provides protection for those who have been recently vaccinated or who received it in the past.
- Monkeypox-Specific Vaccine: Research is ongoing into vaccines specifically targeting monkeypox, with several candidates showing promise in trials.
Vaccination Recommendations
Public health authorities recommend vaccination for:
- Healthcare Workers: Individuals who are at higher risk due to their profession.
- High-Risk Populations: People in areas experiencing outbreaks or those with frequent exposure to infected individuals.
Preventive Measures
In addition to vaccination, preventive measures include:
- Good Hygiene: Regular handwashing and use of hand sanitizers.
- Avoiding Contact: Minimizing close contact with individuals displaying symptoms or with infected animals.
- Isolation: Infected individuals should isolate themselves to prevent the spread of the virus.
Conclusion
The emergence of Monkeypox Clade 1b represents a significant challenge to global health. Its increased transmissibility and potential for severe outcomes highlight the importance of staying informed and proactive.
By understanding its transmission, symptoms, and preventive measures, individuals and communities can better protect themselves and mitigate the impact of this new strain.
FAQs
1. What makes Clade 1b different from other monkeypox strains?
Clade 1b is noted for its increased transmissibility and potentially more severe outcomes compared to other strains.
It spreads faster and may lead to more serious health issues, necessitating closer monitoring and enhanced preventive measures.
2. How can I tell if I have monkeypox or another viral infection?
Monkeypox often begins with flu-like symptoms and progresses to a distinct rash.
If you experience these symptoms, especially if you’ve been in contact with someone who has monkeypox or are in an outbreak area, seek medical advice for accurate diagnosis and testing.
3. Is the smallpox vaccine effective against Monkeypox Clade 1b?
Yes, the smallpox vaccine offers protection against monkeypox, including Clade 1b, due to the similarities between the two viruses.
However, its effectiveness may vary based on factors such as time since vaccination and individual health conditions.
4. Are there any new vaccines specifically for monkeypox?
Research is ongoing to develop and approve vaccines specifically targeting monkeypox.
Several candidates are in various stages of clinical trials, with some showing promising results in enhancing protection against monkeypox strains, including Clade 1b.
5. What should I do if I suspect I have monkeypox?
If you suspect you have monkeypox, contact a healthcare provider immediately. They can guide you through testing, diagnosis, and appropriate care.
In the meantime, practice good hygiene and avoid close contact with others to prevent spreading the virus.
References:
Health
Understanding the Low Risk of Mpox Outbreak in India and Our Preparedness Measures

-

 Trending Stories1 year ago
Trending Stories1 year agoCDC: 1 in 4 Americans Still COVID-Free by End of 2022
-

 Health5 years ago
Health5 years agoMeghan Trainor Shares Motivational New Song ‘Blink’
-

 Health2 years ago
Health2 years agoHow Long Does Monkey Pox Last Before It Surfaces in the Body?
-

 Health2 years ago
Health2 years agoWhat Causes Swollen Body? Understanding Edema and its Triggers
-

 Health4 months ago
Health4 months agoHow Do Pawpaw Seeds Support Cardiovascular Health?
-

 Health3 years ago
Health3 years agoNutrition and the Importance of a Fitness Program – 3 Things to Know
-

 Health3 years ago
Health3 years ago5 Weird Reasons Why Pimples Disappear After Marriage
-

 Health2 years ago
Health2 years agoHealth Benefits Of Pawpaw Seed? 7 Things To Know